This 2022 edition of Death on the Job: The Toll of Neglect marks the 31st year the AFL-CIO has produced a report on the state of safety and health protections for America’s workers. This report features national and state information on workplace fatalities, injuries and illnesses, as well as the workplace safety inspections, penalties, funding, staffing and public employee coverage under the Occupational Safety and Health Act. It also includes information on the state of mine safety and health and the state of worker safety during the COVID-19 pandemic.
Fifty-one years ago on April 28, the OSH Act went into effect, promising every worker the right to a safe job. More than 647,000 workers now can say their lives have been saved since the passage of the OSH Act.¹ Since that time, workplace safety and health conditions have improved. But too many workers remain at serious risk of injury, illness or death as chemical plant explosions, major fires, construction collapses, infectious disease outbreaks, workplace assaults and other preventable workplace tragedies continue to occur. Workplace hazards kill and disable approximately 125,000 workers each year—4,764 from traumatic injuries, and an estimated 120,000 from occupational diseases. Job injury and illness numbers continue to be severe undercounts of the real problem.
Over the years, our progress has become more challenging as employers’ opposition to workers’ rights and protections has grown, and attacks on unions have intensified. Big Business and many Republicans have launched an aggressive assault on worker protections. They are attempting to shift employers’ responsibility to maintain a safe workplace to individual worker behavior, and undermine the core responsibilities of workplace safety agencies.
The Trump administration rolled back progress, attacking longstanding workplace safety protections—targeting job safety rules on beryllium, mine safety examinations and injury reporting, and cutting agency budgets and staff—and attempted to dismantle the systems for future protections. They totally failed to respond to the COVID-19 pandemic and the disparities of those most affected by workplace infection.
In the fall of 2019, the Occupational Safety and Health Administration (OSHA) began reducing the number of inspections involving significant cases and complex health hazards, a policy that is still in place today. In the first year of the COVID-19 pandemic, OSHA was largely absent from workplaces where it has the authority and responsibility to enforce workplace safety laws. While the number of inspectors and inspections have improved in FY 2021, there is much more progress to be made to meet or exceed pre-pandemic levels. The COVID-19 pandemic also brought to light the weaknesses in federal oversight of state OSHA plans. Congress continues to fund job safety at stagnant levels, allowing an OSHA budget that still only amounts to $4.37 to protect each worker covered by the OSH Act.
While progress is slow, the Biden administration has taken important steps to protect workers, prioritizing worker protections on its regulatory agenda, taking steps on targeted enforcement efforts on urgent hazards, and filling staff and leadership vacancies. It also launched broad efforts on worker empowerment and targeting workplace inequities.
President Joe Biden has appointed and nominated strong candidates focused on worker protection to lead job safety and health agencies and labor agencies. Immediately upon taking office, he appointed a longtime United Steelworkers (USW) safety and health leader, James Frederick, as acting assistant secretary for occupational safety and health. In April 2021, the Senate confirmed Marty Walsh, the Boston mayor from the construction trades unions, as secretary of labor. In April 2021, Biden nominated Doug Parker to be assistant secretary of labor for occupational safety and health—the head of OSHA—and he was confirmed Oct. 25, 2021.
Parker served as the California OSHA chief, on the Biden-Harris transition team, in chief policy roles at the Mine Safety and Health Administration (MSHA) and was executive director of Worksafe—a nonprofit organization focused on workplace injury, illness and death prevention. John Howard continues to serve as the head of the National Institute for Occupational Safety and Health (NIOSH). This is a sharp contrast to President Donald Trump, who nominated corporate officials to head the job safety agencies—people who had records of opposing enforcement and regulatory actions, and who often lacked safety experience.
Executive Summary
This 2022 edition of “Death on the Job: The Toll of Neglect” marks the 31st year the AFL-CIO has produced a report on the state of safety and health protections for America’s workers. The Occupational Safety and Health Act, promising every worker the right to a safe job, has been in effect for more than 50 years, and more than 647,000 workers now can say their lives have been saved since the passage of the OSH Act.
Over the last 50 years, there has been significant progress toward improving working conditions and protecting workers from job injuries, illnesses and deaths. Federal job safety agencies have issued many important regulations on safety hazards and silica, coal dust and other health hazards, strengthened enforcement and expanded worker rights.
These initiatives have undoubtedly made workplaces safer and saved lives. But much more progress is needed.
Over the years, the progress has become more challenging as employers’ opposition to workers’ rights and protections has grown, and attacks on unions have intensified. Big Business and many Republicans have launched an aggressive assault on worker protections. They are attempting to shift employers’ responsibilities to provide safe jobs to individual workers, and undermine the core responsibilities of workplace safety agencies.
The nation must renew its commitment to protecting workers from job injury, disease and death, and make this a high priority. Employers must meet their responsibilities to protect workers and be held accountable if they put workers in danger. Only then can the promise of safe jobs for all of America’s workers be fulfilled. There is much more work to be done to ensure the fundamental right to a safe job is a reality for all.
The High Toll of Job Injuries, Illnesses and Deaths
In 2020:
- 340 workers died each day from hazardous working conditions.
- 4,764 workers were killed on the job in the United States.
- An estimated 120,000 workers died from occupational diseases.
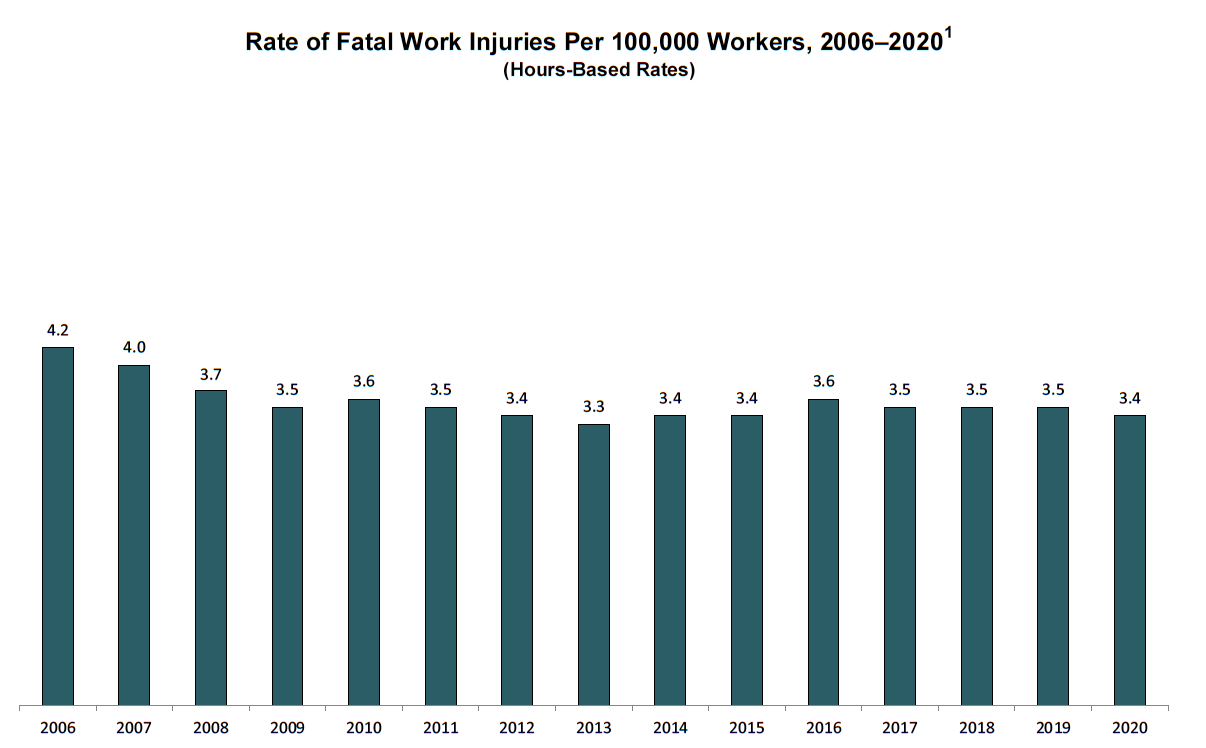
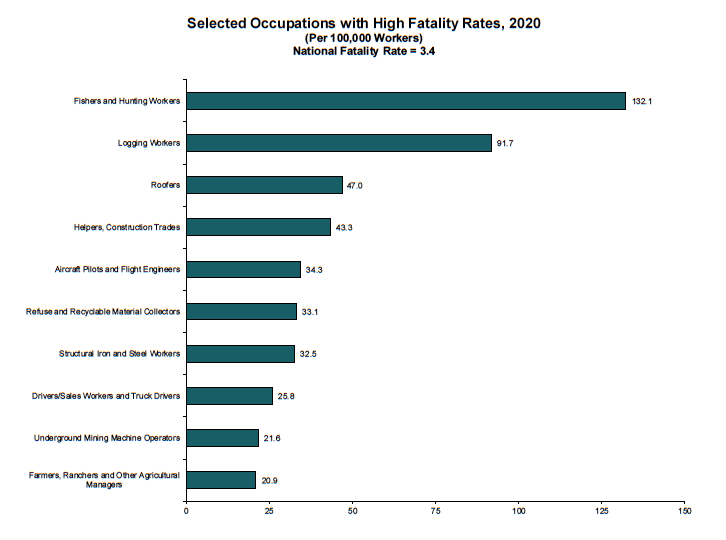
- The job fatality rate was 3.4 per 100,000 workers.
- Latino and Black workers remain at greater risk of dying on the job than all workers.
- Employers reported nearly 3.2 million work-related injuries and illnesses.
- Musculoskeletal disorders continue to make up the largest portion (21%) of work- related injuries and illnesses.
- Underreporting is widespread—the true toll of work-related injuries and illnesses is 5.4 million to 8.1 million each year.
The cost of job injuries and illnesses is enormous—estimated at $176 billion to $352 billion a year.
States with the highest fatality rates in 2020 were:
- Wyoming (13.0 per 100,000 workers)
- Alaska (10.7 per 100,000 workers)
- South Dakota (7.8 per 100,000 workers)
- North Dakota (7.4 per 100,000 workers)
- West Virginia (6.6 per 100,000 workers)
Industries with the highest fatality rates in 2020 were:
- Agriculture, forestry, and fishing and hunting (21.5 per 100,000 workers)
- Transportation and warehousing (13.4 per 100,000 workers)
- Mining, quarrying, and oil and gas extraction (10.5 per 100,000 workers)
- Construction (10.2 per 100,000 workers)
- Wholesale trade (4.6 per 100,000 workers)c
Latino and Black workers, often laboring in dangerous working conditions, are more likely to die on the job:
- The Latino fatality rate increased again to 4.5 per 100,000 workers in 2020, 32% greater than the national average; that marks a 15% increase over the past decade.
- The number of Latino worker deaths in 2020 was similar to the previous year: 1,072 deaths in 2020, compared with 1,088 in 2019. Of those who died in 2020, 65% were immigrants.
- The Black worker fatality rate of 3.5 per 100,000 workers continues to be greater than the national average.
- 541 Black workers died on the job, a decrease from 2019.
Older workers are at high risk. In 2020:
- More than one-third of workplace fatalities occurred among workers ages 55 and older.
- Workers 65 and older have 2.5 times the risk of dying on the job as other workers, with a fatality rate of 8.6 per 100,000 workers.
During the COVID-19 pandemic:
- America’s workplaces are a primary source of COVID-19 outbreaks, with thousands of workers infected and dying as they work in indoor, poorly ventilated spaces. However, workplace infection and outbreak information is limited because there is no national data surveillance system.
- Racial inequities in working conditions, disease and death were made worse and exploited.
- The federal Occupational Safety and Health Administration (OSHA) issued a COVID- 19 emergency temporary standard for health care (ETS for health care) on June 21, 2021. This provided health care workers with enforceable protections against exposure to the virus at work. On Dec. 27, 2021, OSHA announced a plan to withdraw the emergency standard and focus on permanent protections, leaving health care workers without COVID-19 protections in the meantime, including during the Omicron surge.
- All other workers have worked throughout the pandemic with only unenforceable guidance by federal OSHA. Recommendations from the Centers for Disease Control and Prevention (CDC) are weak, insufficient and have changed frequently within these two years, and have been plagued with political interference and corporate influence.
- Federal OSHA so far has issued 2,507 COVID-19-related violations, including 203 ETS for health care citations, 26 5(a)(1) citations, as well as respiratory protection, personal protective equipment and recordkeeping citations. The average penalty for a COVID-19-related violation was $3,281 per violation.
- Several state OSHA plans issued emergency temporary standards for COVID-19, and other states have issued executive orders requiring employers to implement workplace safety protections, or are enforcing current OSHA standards in their states—but many of these actions have been revoked or weakened as variants continue to spread in workplaces.
Workplace violence remains a serious and growing problem:
- Workplace violence deaths increased to 705 in 2020, while more than 27,000 violence- related lost-time injuries were reported.
- 392 worker deaths were workplace homicides.
- Workplace violence is the fourth-leading cause of workplace death overall and the second-leading cause of workplace death for women.
- Women workers are at greater risk of violence than men; they suffer seven of every 10 lost-time injuries related to workplace violence, and are 50% more likely to be killed by a relative or domestic partner in the workplace than men.
- There is no federal OSHA standard to protect workers from workplace violence.
Job Safety Oversight and Enforcement
OSHA resources in FY 2021 still are too few to be a deterrent:
- There are only 1,719 inspectors (755 federal and 964 state) to inspect the 10.4 million workplaces under the Occupational Safety and Health Act’s jurisdiction.
- The number of OSHA inspectors is near its lowest number since the agency opened more than 50 years ago.
- There is one inspector for every 81,427 workers.
- The current OSHA budget amounts to $4.37 to protect each worker.
Penalties in FY 2021 still are too weak:
- The average penalty for a serious violation was $4,460 for federal OSHA.
- The average penalty for a serious violation was $2,421 for OSHA state plans.
- The median penalty for killing a worker was $9,753 for federal OSHA.
- The median penalty for killing a worker was $5,825 for state OSHA plans.
- Only 115 worker death cases have been criminally prosecuted under the Occupational Safety and Health Act since 1970.
Much Work Remains to Be Done
Workers need more job safety and health protection, not less. We call on:
- OSHA and the Mine Safety and Health Administration (MSHA) to fully enforce job safety and health protections to hold employers accountable for not following workplace safety and health laws, and federal OSHA to strengthen oversight of state OSHA plans.
- OSHA to increase attention to the significant safety and health problems faced by Latino, Black, immigrant and aging workers, and those under other work arrangements.
- OSHA and MSHA to strengthen anti-retaliation protections and worker participation rights.
- OSHA to expeditiously issue a permanent COVID-19 standard to protect health care workers from airborne and other routes of exposure, and require employers to protect other workers in congregate work settings, such as in food processing and other manufacturing, corrections and transit.
- OSHA to issue a workplace violence standard for health care and social service workers. The Senate should pass legislation to ensure this is done.
- OSHA to develop and issue new protections and initiatives to address emergency response, heat illness and injury, combustible dust and musculoskeletal disorders.
- MSHA to develop and issue a rule on silica in mining and finalize protections on powered haulage equipment.
- The Environmental Protection Agency to fully implement the Toxic Substances Control Act to protect workers from chemical exposures, coordinating with OSHA and the National Institute for Occupational Safety and Health.
- Congress to increase funding and staffing at job safety agencies, modernizing the stagnant budget that has prevented agencies from fulfilling their obligations.
- Congress to pass the Protecting America’s Workers Act to extend the Occupational Safety and Health Act’s coverage to workers currently excluded, strengthen civil and criminal penalties for violations, enhance anti-discrimination protections, and strengthen the rights of workers, unions and those who have been injured or made ill because of their jobs.
- Elected leaders to oppose Big Business’s regulatory “reform” efforts and legislation that would make it more difficult—or impossible—for agencies to issue needed safeguards.
What Needs to be Done
Over the more than 50 years since the passage of the OSH Act, there has been significant progress made toward improving working conditions and protecting workers from job injuries, illnesses and deaths, preventing devastating losses to working families and saving lives. Federal job safety agencies have issued important regulations on many safety hazards, as well as on silica, coal dust and other health hazards, strengthened enforcement and expanded worker rights. These initiatives undoubtedly have made workplaces safer and saved lives. But much more progress is needed.
The pandemic exposed the regulatory safety and health structural systems that had been weakened over decades and exploited by the Trump administration. Job safety agencies need to be rebuilt, not only restored to the pre-Trump era, but in ways that reflect solutions to the most significant barriers to ensuring workers are protected and can fully exercise their rights. This requires refocusing national attention, energy and action on the enormous role and impact these agencies play to provide workplace oversight and prevent the disease, injuries and death that plague working people across the country. After years of starved budgets, funding and staffing for job safety agencies, and decades of allocating an agency with an extensive mission— OSHA—too few resources, there must be new dedication to substantially increase resources to protect workers, and address ongoing and emerging safety and health problems.
Employers and elected leaders must recognize that employment is a significant determinant of health—and our government must emphasize workplace exposure control measures to resolve this. Severe inequities in dangerous working conditions have created an unacceptable discrepancy in those who face the largest burdens of disease, injury and death because of their jobs. Initiatives to address the safety and health risks posed by changes in the workforce and employment arrangements must take more prominence, and workplace safety and health
regulations must be seen as a significant tool to raise the level of working conditions for those disproportionately affected. There must be renewed, dedicated attention given to the increased risk of fatalities and injuries faced by workers of color and immigrant workers, and aging workers, and enhanced efforts to protect temporary and contract workers.
OSHA must immediately issue a permanent standard to protect health care and other workers in congregate settings from COVID-19. The agency needs to fully enforce this standard and other workplace safety laws by developing a proactive enforcement plan across industries, fully investigating complaints, performing on-site inspections, issuing violations and penalties that reflect the size and scope of the real problem and that deter other employers, and ensure workers’ rights to report unsafe working conditions and refuse dangerous work.
OSHA must swiftly finalize its proposed standard on electronic injury reporting, make more of the data collected public and fully enforce the anti-retaliation protections for workers who report injuries. OSHA must move forward to issue proposed rules on emergency response, heat illness prevention and infectious disease.
Workplace violence is a growing and serious threat, particularly to women workers and those in the health care and social services sectors. OSHA must develop and issue a workplace violence standard, and the Senate should pass the Workplace Violence Prevention for Health Care and Social Service Workers Act to ensure this is done.
OSHA standards for chemical hazards are obsolete and must be updated. The Environmental Protection Agency (EPA) must fully implement the new toxic chemicals reform law and coordinate with OSHA and NIOSH, taking action to address the risks to the public and to workers. New initiatives are needed to address musculoskeletal disorders and combustible dust.
In mining, MSHA must continue initiatives to focus increased attention on mines with a record of repeated violations and stronger enforcement action against mines with patterns of violations. The agency must fully enforce the coal dust rule and act swiftly on new rules on silica and proximity detection for mobile equipment. Congress must strengthen job safety laws to prevent tragedies like the Massey Upper Big Branch mining disaster, which killed 29 miners in West Virginia. Improvements in the Mine Safety and Health Act are needed to give MSHA more authority to shut down dangerous mines and to enhance enforcement against repeat violators.
The Occupational Safety and Health Act now is more than 50 years old and is out of date. Congress must pass the Protecting America’s Workers Act to extend the law’s coverage to workers currently excluded, strengthen civil and criminal penalties for violations, and strengthen the rights of workers and their representatives. Improvements to update and strengthen the OSH Act’s anti-retaliation provisions are particularly needed, so workers can report job hazards and injuries, and exercise safety and health rights without fear.
The nation must renew its commitment to protect workers from injury, disease and death, and make this a high priority. We must demand that employers meet their responsibilities to protect workers and hold them accountable if they put workers in danger. Only then can the promise of safe jobs for all of America’s workers be fulfilled.
1 Calculated based on changes in annual fatality rates and employment since 1970. Fatality rate data for 1970 to 1991 is from National Safety Council Accident Facts, 1994. Fatality rate data for 1992 to 2020 is from the Bureau of Labor Statistics, Census of Fatal Occupational Injuries. Annual employment data is from the Bureau of Labor Statistics Current Population Survey.
2 U.S. Department of Labor, Bureau of Labor Statistics, Census of Fatal Occupational Injuries, 2020.
3 Takala, J., P. Hämäläinen, N. Nenonen, et al. “Comparative Analysis of the Burden of Injury and Illness at Work in Selected Countries and Regions,” Central European Journal of Occupational and Environmental Hygiene 23:1– 2, 6–31, (2017). icohweb.org/site/images/news/pdf/CEJOEM%20Comparative%20analysis%20published%2023_1- 2_Article_01.pdf.
4 Liberty Mutual Research Institute for Safety, news release, April 16, 2002.
5 Leigh, J.P. “Economic Burden of Occupational Injury and Illness in the United States.” The Milbank Quarterly 89, No. 4. December 2011. Available at 10.1111/j.1468-0009.2011.00648.x
Job Fatalities
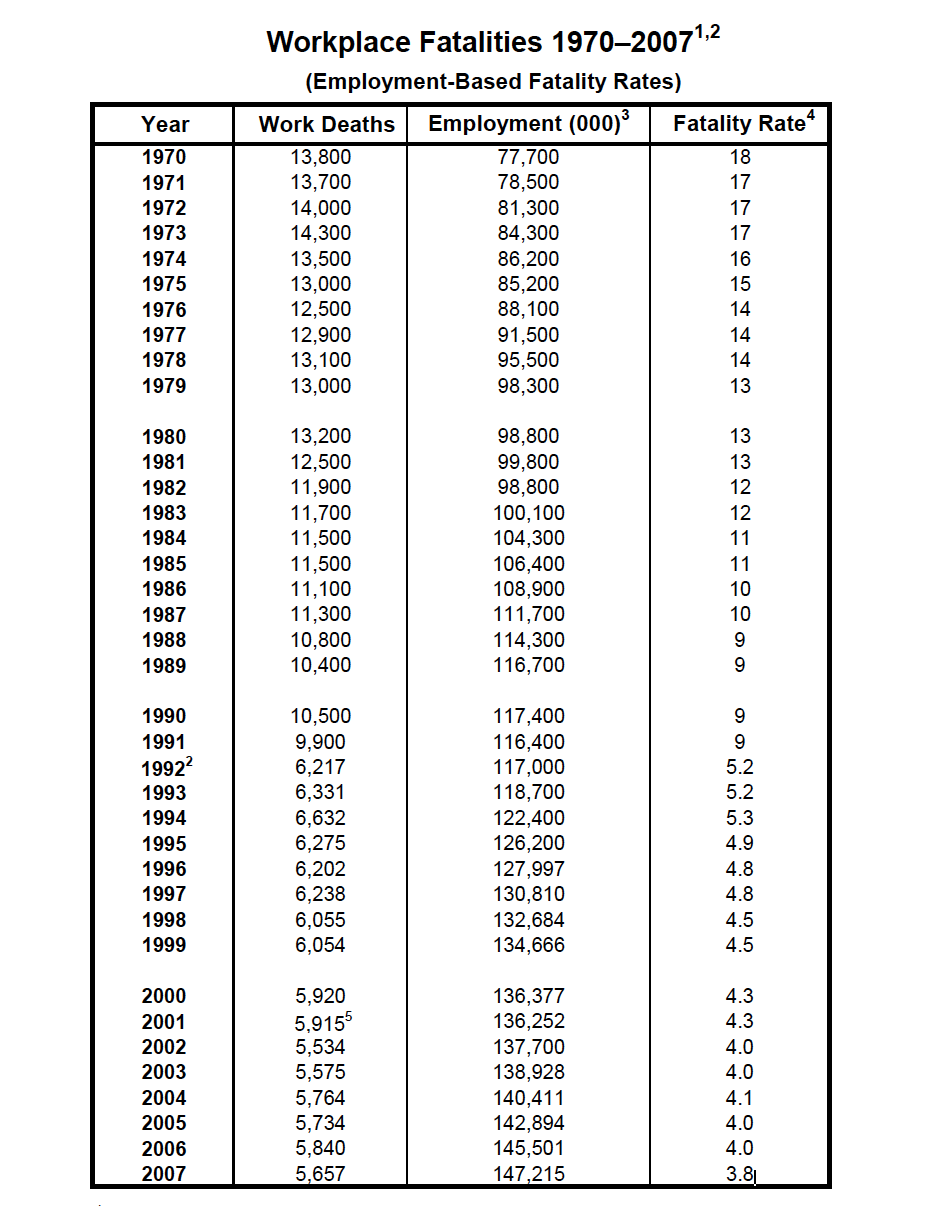
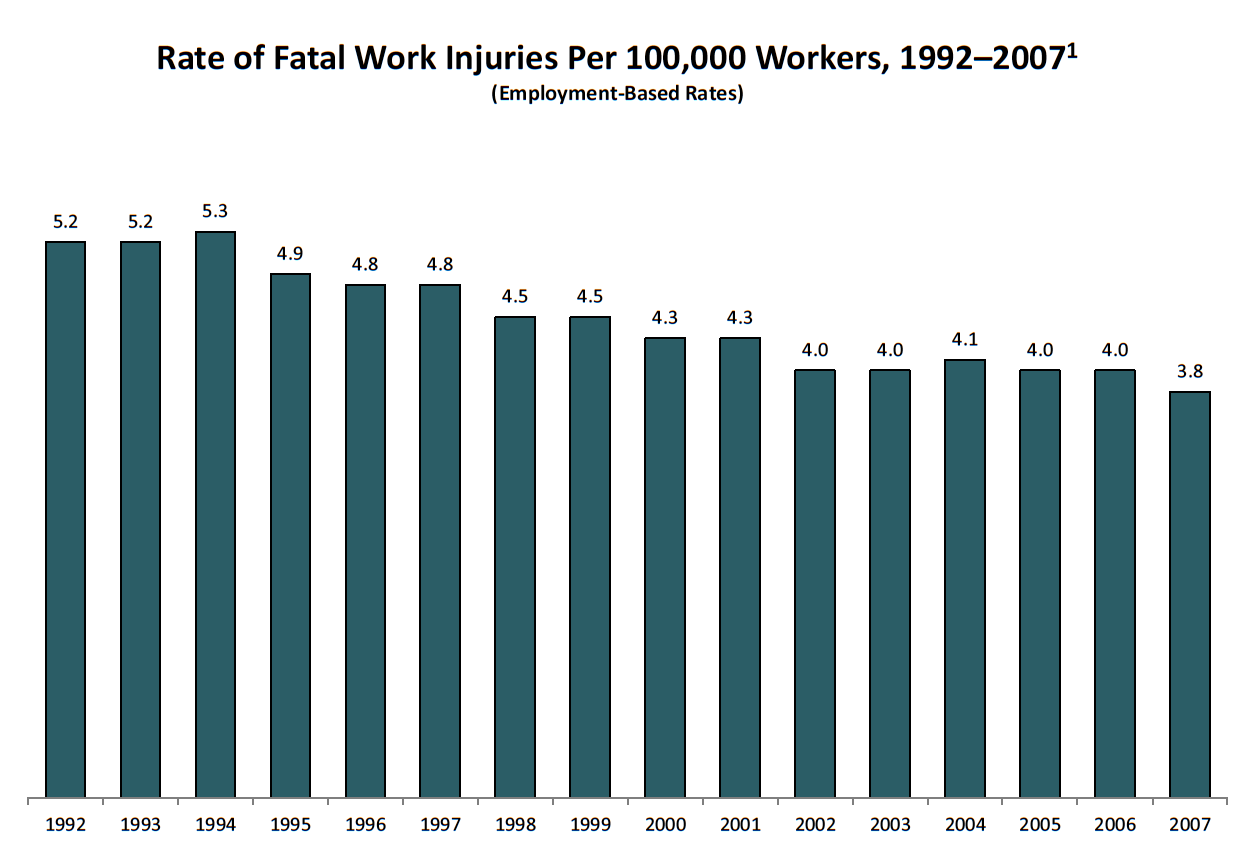
In 2020, 4,764 workers lost their lives on the job as a result of traumatic injuries, an increase from 2018, according to fatality data from the Bureau of Labor Statistics (BLS). The rate of fatal job injuries in 2020 was 3.4 per 100,000 workers, the first decrease in years.² Each day in this country, an average of 15 workers die because of job injuries—women and men who go to work, never to return home to their families and loved ones. This does not include workers who die from occupational diseases, estimated to be 120,000 each year.³ This number does not include the many thousands who died from being exposed to COVID-19 at work. Chronic occupational diseases receive less attention and place little accountability on employers because most are not detected until years after workers have been exposed to toxic chemicals and other agents, and because occupational illnesses often are misdiagnosed and poorly tracked. There is no national comprehensive surveillance system for occupational illnesses. In total, about 340 workers die each day due to job injuries and illnesses. The cost of these injuries and illnesses is enormous— estimated at $176 billion to $352 billion a year.⁴⁵
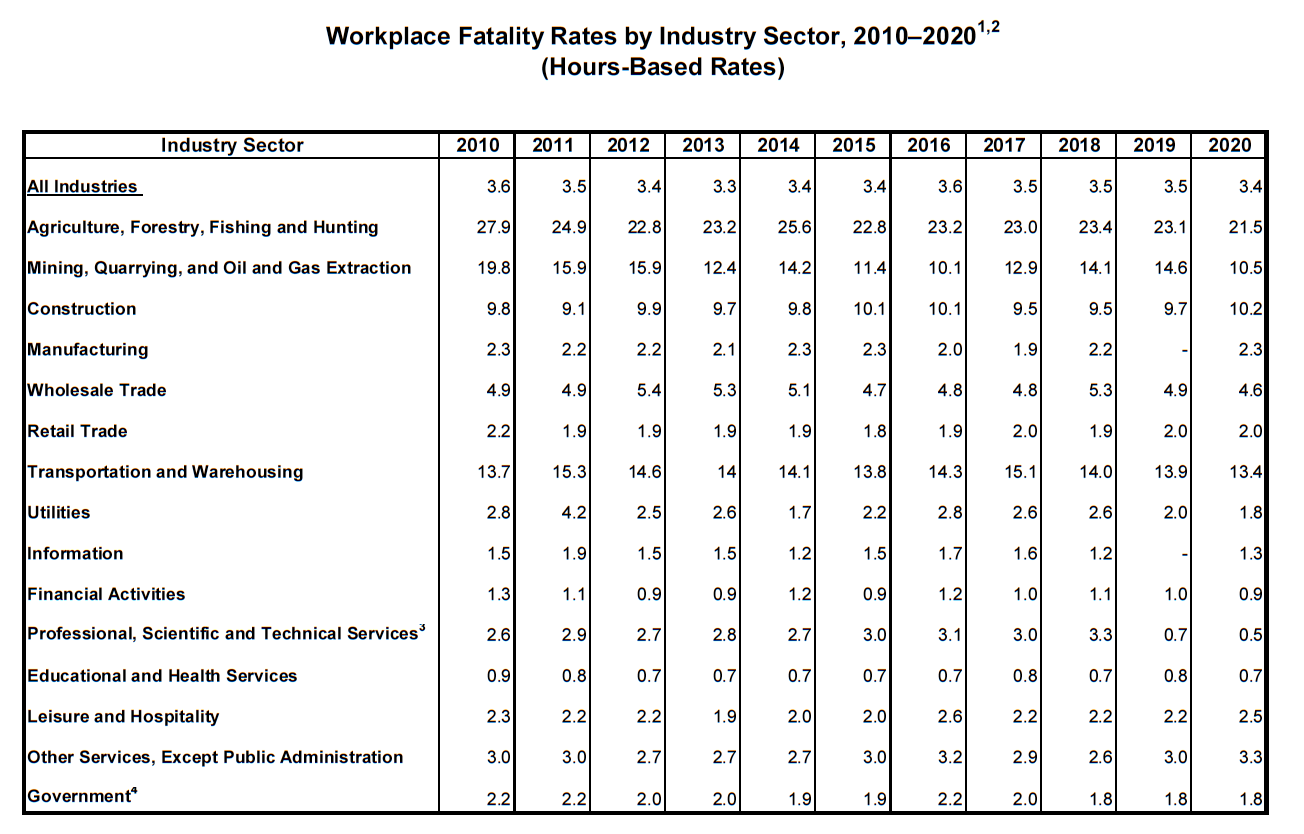
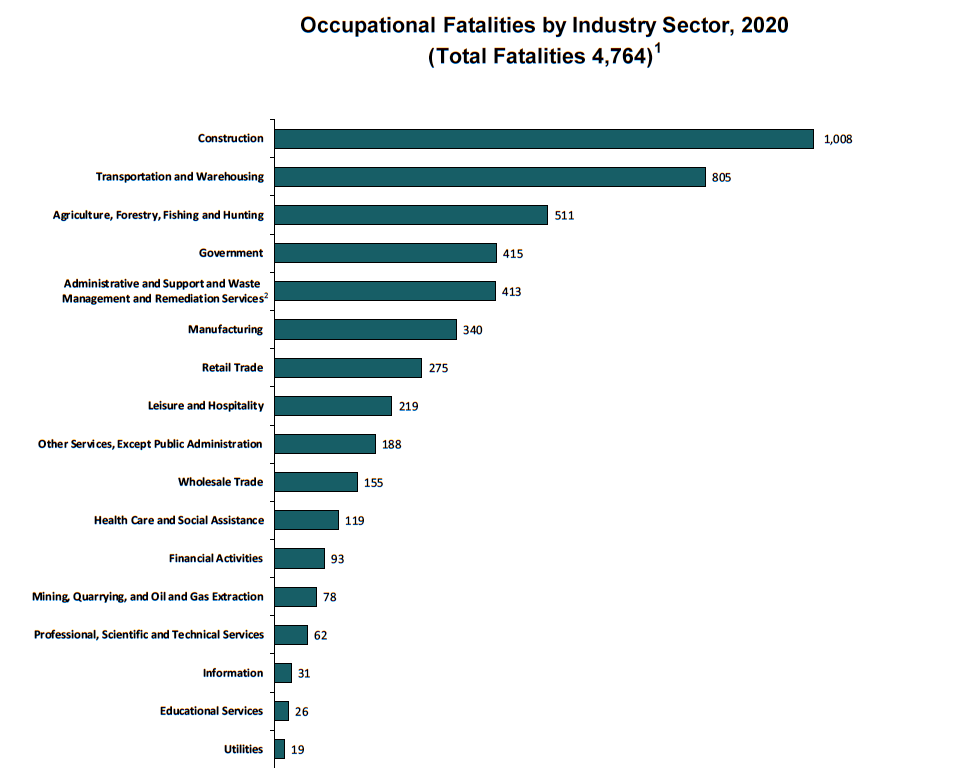
In 2020, agriculture, forestry, and fishing and hunting continues to be the most dangerous industry (21.5 deaths per 100,000 workers), followed by transportation and warehousing (13.4 per 100,000 workers), mining, quarrying, and oil and gas extraction (10.5 per 100,000 workers), construction (10.2 per 100,000 workers) and wholesale trade (4.6 per 100,000 workers).
Transportation incidents, in particular roadway crashes, continue to be the leading cause of workplace deaths, responsible for 1,778 or 37% of all fatalities in 2020, followed by deaths from falls, slips and trips (805, or 16.9%) and contact with objects and equipment (716, or 15%).
The job fatality rate for all self-employed workers—a group that lacks OSHA coverage— continues to remain high at 12.3 per 100,000 workers, more than four times the rate among wage and salary workers (2.9 per 100,000). In 2020, 900 contract workers died on the job—19% of all worker deaths. BLS had begun reporting details on fatalities that involve workers employed as contractors in 2012 in response to concerns about safety and health issues among these workers. Fatality data in 2019 and forward no longer report details of contractor deaths due to a 2020 BLS policy on disclosure methodology and reduction in publishable data—pulling back on transparency of details among contract worker deaths.
States with the highest fatality rates include Wyoming (13.0 per 100,000 workers), Alaska (10.7 per 100,000 workers), South Dakota (7.8 per 100,000 workers), North Dakota (7.4 per 100,000 workers) and West Virginia (6.6 per 100,000 workers). In 2020, despite the overall job fatality rate decrease, the job fatality rate increased in 20 states, compared with 2019.
1Fatality information for 1971 to 1991 from National Safety Council Accident Facts, 1994.
2 Fatality information for 1992 to 2007 is from the Bureau of Labor Statistics, Census of Fatal Occupational Injuries. In 1994, the National Safety Council changed its reporting fatalities and adopted the BLS count. The earlier NSC numbers are based on an estimate; the BLS method for workplace numbers are based on an actual census.
3 Employment is an annual average of employed civilians 16 years of age and older from the Current Population Survey, adjusted to include data for resident and armed forces from the Department of Defense.
4 Deaths per 100,000 workers are based on annual average of employed civilians 16 years of age and older from 1992 to 2007. In 2008, CFOI switched from an employment-based fatality rate to an hours-based fatality rate calculation. Employment-based fatality rates should not be compared with hours-based fatality rates.
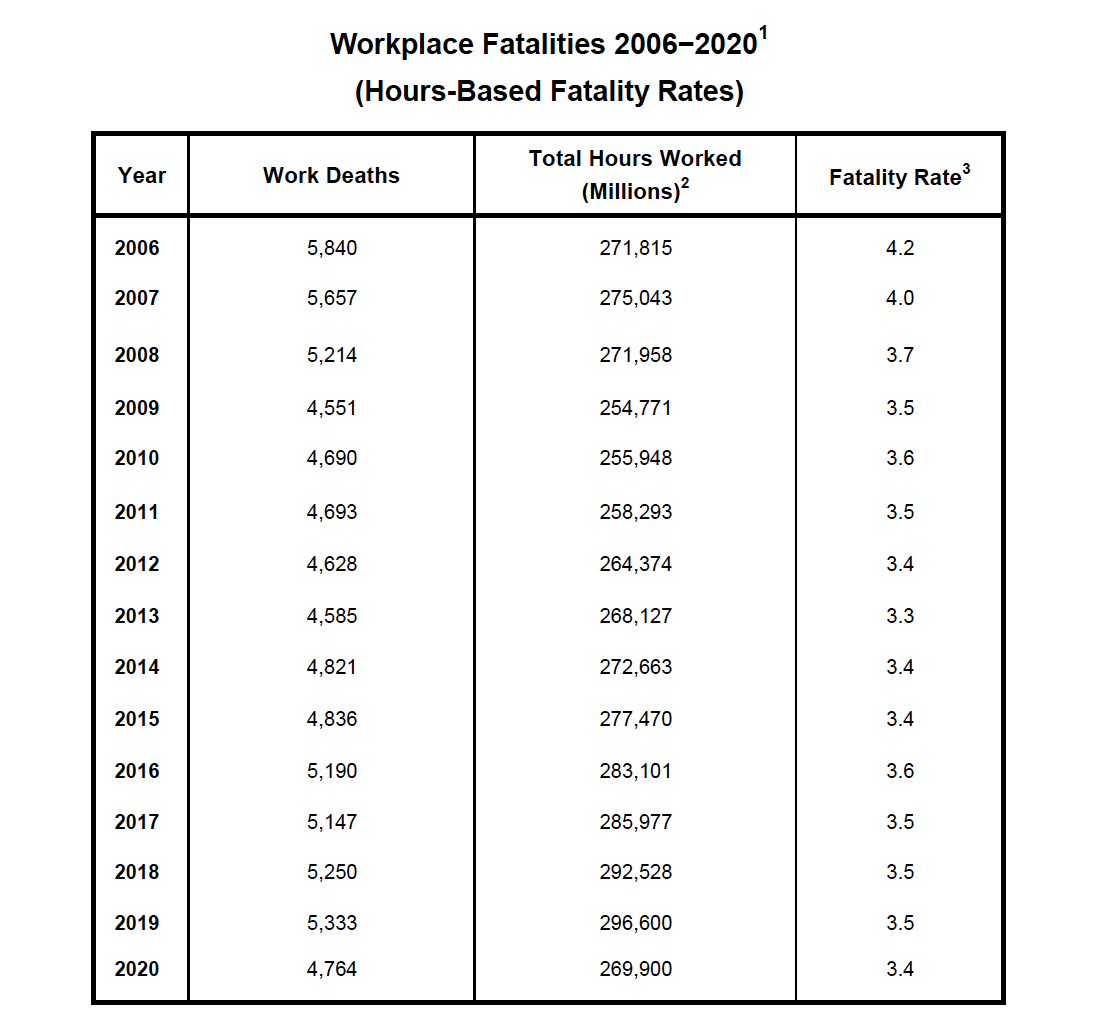
1 Fatality information is from the U.S. Department of Labor, Bureau of Labor Statistics, Census of Fatal Occupational Injuries.
2 The total hours worked figures are annual average estimates of total persons at work multiplied by average hours for civilians, 16 years of age and older, from the Current Population Survey, U.S. Bureau of Labor Statistics.
3 Deaths per 100,000 workers. In 2008, CFOI switched to an hours-based fatality rate calculation from an employment-based calculation used from 1992 to 2007. Fatality rates for 2006 and 2007 were calculated by CFOI using both approaches during the transition to hours-based rates beginning exclusively in 2008. Hours-based fatality rates should not be compared directly with the employment-based rates CFOI calculated for 1992 to 2007.
Sources: U.S. Department of Labor, Bureau of Labor Statistics, Current Population Survey, Census of Fatal Occupational Injuries; U.S. Bureau of the Census; and U.S. Department of Defense.
1 Incidence rate represents the number of fatalities per 100,000 workers. Fatality rate is an employment-based calculation using employment figures that are annual average estimates of employed civilians, 16 years of age and older, from the Current Population Survey, U.S. Bureau of of Labor Statistics. In 2008, CFOI switched to an hours-based fatality rate calculation. Employment-based fatality rates should not be compared directly with hours-based rates.
Source: U.S. Department of Labor, Bureau of Labor Statistics, Census of Fatal Occupational Injuries.
1 Incidence rate represents the number of fatalities per 100,000 workers. Fatality rate is an hours-based calculation using total hours worked figures that are annual average estimates of total persons at work multiplied by average hours for civilians, 16 years of age and older, from the Current Population Survey, U.S. Bureau of Labor Statistics. Hours-based fatality rates should not be compared directly with the employment-based rates CFOI calculated for 1992 to 2007.
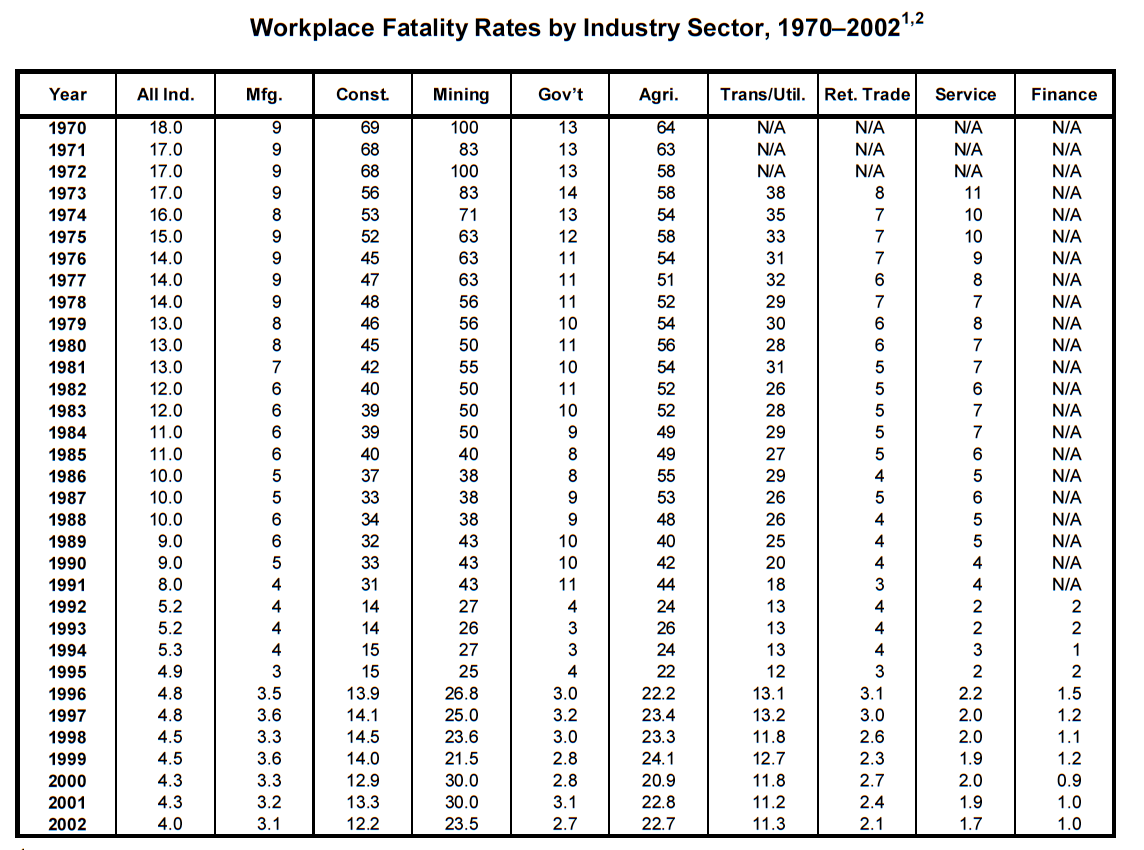
1 Data for 1970–1991 is from the National Safety Council, Accident Facts, 1994. Fatality information for 1992–2002 is from the Bureau of Labor Statistics, Census of Fatal Occupational Injuries. In 1994, the National Safety Council changed its reporting method for workplace fatalities and adopted the BLS count. The earlier NSC numbers are based on an estimate; the BLS numbers are based on an actual census. Beginning with 2003, CFOI began using the North American Industry Classification for industries. Prior to 2003, CFOI used the Standard Industrial Classification system. The substantial differences between these systems result in breaks in series for industry data.
2 Deaths per 100,000 workers.
Source: U.S. Department of Labor, Bureau of Labor Statistics, Census of Fatal Occupational Injuries.
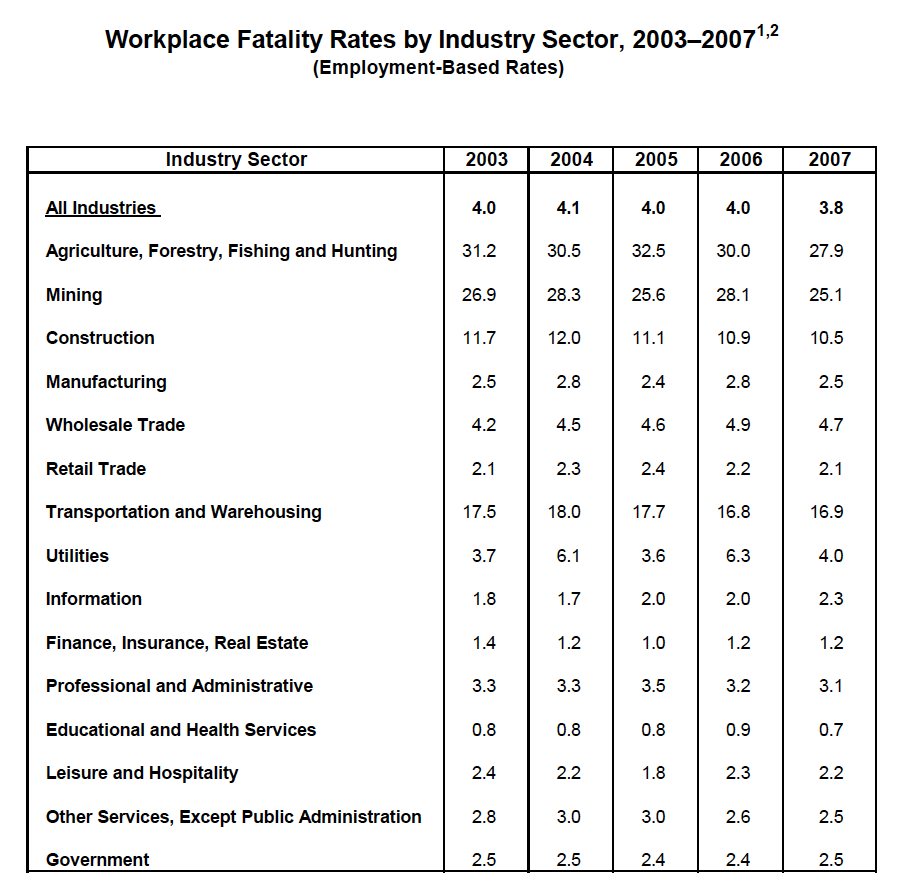
1 Deaths per 100,000 workers.
2 Fatality rate is an employment-based calculation using employment figures that are annual average estimates of employed civilians, 16 years of age and older, from the Current Population Survey. In 2008, CFOI switched to an hours-based fatality rate calculation.
Employment-based fatality rates should not be compared directly with hours-based rates.
Note: Beginning with the 2003 reference year, both CFOI and the Survey of Occupational Injuries and Illnesses began using the 2002 North American Industry Classification System (NAICS) for industries. Prior to 2003, the surveys used the Standard Industrial Classification (SIC) system. The substantial differences between these systems result in breaks in series for industry data.
Source: U.S. Department of Labor, Bureau of Labor Statistics, Census of Fatal Occupational Injuries.
1 Deaths per 100,000 workers.
2Fatality rate is an hours-based calculation uisng total hours worked figures that are annual average estimates of total persons at work multiplied by average hours for civilians, 16 years of age and older, from the Current Population Survey. Hours-based fatality rates should not be compared directly with employment-based rates that CFOI calculated for 1992 to 2007.
3 In this sector, landscaping services had a fatality rate of 17.9 and waste management services and remediation services had a fatality rate of 15.0 in 2020.
4 Government fatalities may overlap with specific industry sectors listed.
Source: U.S. Bureau of Labor Statistics, U.S. Department of Labor.
Note: Oil and gas extraction industries include oil and gas extraction (NAICS 21111), drilling oil and gas wells (NAICS 213111), and support activities for oil and gas operations (NAICS 213112).
Source: U.S. Department of Labor, Bureau of Labor Statistics, Census of Fatal Occupational Injuries.
Workplace Injuries and Illnesses are Underreported and Costly
Nonfatal Injuries and Illnesses
In 2020, nearly 3.2 million workers across all industries, including state and local government, had work-related injuries and illnesses that were reported by employers, with 2.7 million injuries and illnesses reported in private industry. In 2020, state and local public sector employers reported an injury rate of 3.9 per 100 workers, 44% higher than the reported rate of 2.7 per 100 among private sector workers.⁶
Due to limitations in the current injury reporting system and widespread underreporting of workplace injuries, this number understates the problem. The true toll is estimated to be two to three times greater—or 5.4 million to 8.1 million injuries and illnesses a year. In addition, states are not required to report to BLS; its Survey of Occupational Injuries and Illnesses is voluntary.
The number of reported illnesses in private industry, including COVID-19, more than quadrupled in 2020 to 544,600 illnesses, compared with 127,200 in 2019. This is not a true count of occupational COVID-19 illness. However, studies have not been done to determine the number of cases of all work-related illnesses, and recently, work-related COVID-19, have been missed by the survey. This estimate is likely much greater given other documentation throughout the pandemic.
Reported Cases Understate the Problem
Over the last decade, there has been significant research documenting that the BLS survey fails to capture a large proportion of work-related injuries and illnesses—one-third to two-thirds of work-related injuries and illnesses are missed by the survey. Studies comparing injuries captured by the BLS survey with injuries reported to workers’ compensation or other injury reporting systems have found that the BLS survey missed 33% to 69% of work-related injuries.⁷⁸⁹¹⁰ A 2018 study of injury reporting in the mining industry found a similar result. Two-thirds of the injuries among miners in Illinois that were reported to workers’ compensation were not reported to MSHA by mine operators as required by the law.¹¹ A study that compared state fatality rates in the construction industry with rates of injuries that result in lost time or job restriction found
there was little correlation between the two, and in some cases there was a negative correlation.¹² The study observed that multiple factors impacted the reporting and recording of injuries, and concluded that fatality rates are a much more valid measure of risk.
Some of the undercount in the BLS survey is due to injuries excluded from the BLS survey’s scope, including injuries among self-employed individuals, and the design of the survey.¹³ But other factors, including employees’ reluctance to report injuries due to fear of retaliation, incentive programs that penalize workers who report injuries and drug testing programs for workplace injuries, suppress reporting.¹⁴ In addition, there are disincentives for employers to report injuries, which include concern about increased workers’ compensation costs for increased reports of injuries; fear of being denied government contracts due to high injury rates; concern about being targeted by OSHA for inspection if a high injury rate is reported; and the promise of monetary bonuses for low injury rates. A 2020 study by BLS investigating additional causes of underreporting indicated that keeping of injury and illness logs was not widely prevalent, and that small establishments were less likely than mid-sized and large establishments to keep records.¹⁵
BLS also has recognized the need to make changes in its program in order to collect more complete and accurate injury and illness statistics. It launched a pilot of a Household Survey on Occupational Injuries and Illnesses to collect information on work-related injuries and illnesses through interviews with workers.¹⁶ The initial results showed that the survey needed improvements to reduce respondent burden, to improve survey completion and to identify OSHA-recordable injuries, but it has potential to be a supplement to the existing employer-based injury and illness survey. BLS will continue to work on improvements to the survey.¹⁷ A 2018 report from the National Academies of Sciences, Engineering and Medicine on occupational safety and health surveillance strongly endorsed BLS conducting this new household survey.¹⁸ Hopefully, if the pilot is successful, Congress will provide the necessary funding to continue and expand this important work.
6 U.S. Department of Labor, Bureau of Labor Statistics, Survey of Occupational Injuries and Illnesses, 2020.
7 Boden, L.I., and A. Ozonoff. “Capture-Recapture Estimates of Nonfatal Workplace Injuries and Illnesses.” Annals of Epidemiology 18, No. 6. 2008. Available at 10.1016/j.annepidem.2007.11.003.
8 Rosenman, K.D., A. Kalush, M.J. Reilly, et al. “How Much Work-Related Injury and Illness is Missed by the Current National Surveillance System?” Journal of Occupational and Environmental Medicine 48, No. 4, 357–67. April 2006. Available at 10.1097/01.jom.0000205864.81970.63.
9 Davis, L., K. Grattan, S. Tak, et al. “Use of Multiple Data Sources for Surveillance of Work-Related Amputations in Massachusetts, Comparisons with Official Estimates and Implications for National Surveillance.” American Journal of Industrial Medicine 57, No. 10. April 29, 2014. Available at 10.1002/ajim.22327.
10 Wuellner, S., and D. Bonauto. “Injury Classification Agreement in Linked Bureau of Labor Statistics and Workers’ Compensation Data.” American Journal of Industrial Medicine 57, No. 10. Dec. 17, 2013. Available at 10.1002/ajim.22289.
11 Almberg, K.S., L.S. Friedman, D. Swedler and R.A. Cohen. “Mine Safety and Health Administration’s Part 50 program does not fully capture chronic disease and injury in the Illinois mining industry.” American Journal of Industrial Medicine 61, 436–443. March 9, 2018. Available at 10.1002/ajim.22826.
12 Mendeloff, J., and R. Burns. “States with low non‐fatal injury rates have high fatality rates and vice‐versa.” American Journal of Industrial Medicine 56, 509–519. April 2, 2012. Available at 10.1002/ajim.22047 (2013).
13 Wiatrowski, W.J. “Examining the Completeness of Occupational Injury and Illness Data: An Update on Current Research.” Monthly Labor Review. June 2014. Available at BLS.gov/opub/mlr/2014/article/examining-the- completeness-of-occupational-injury-and-illness-data-an-update-on-current-research.htm.
14 United States Government Accountability Office. “Enhancing OSHA’s Records Audit Process Could Improve the Accuracy of Worker Injury and Illness Data.” GAO-10-10. October 15, 2009. Available at GAO.gov/products/GAO-10-10.
15 Rogers, E. “The Survey of Occupational Injuries and Illnesses Respondent Follow-Up Survey.” Monthly Labor Review. U.S. Bureau of Labor Statistics. May 2020. Available at doi.org/10.21916/mlr.2020.9.
16 U.S. Bureau of Labor Statistics. Research on the Completeness of the Injury and Illness Counts from the Survey of Occupational Injuries and Illnesses. Available at BLS.gov/iif/undercount.htm.
17 Yu, E., and K. Monaco. “Overview of the Results of the Household Survey of Occupational Injuries and Illnesses Pilot and On-going BLS Activities.” U.S. Bureau of Labor Statistics. Dec. 5, 2020. Available at BLS.gov/iif/hsoii- update-12052020-final.pdf.
18 National Academies of Sciences, Engineering, and Medicine. A Smarter National Surveillance System for Occupational Safety and Health for the 21st Century. Washington, D.C.: The National Academies Press, (2018). Available at doi.org/10.17226/24835.
Cost of Occupational Injuries and Deaths
The cost of occupational injuries and deaths in the United States is staggering, estimated at $176 billion to $352 billion a year, according to two recent studies.
The 2021 Workplace Safety Index, published by Liberty Mutual Insurance, estimated the cost of the most disabling workplace injuries to employers at more than $58 billion a year—more than $1 billion per week.¹⁹ This analysis, based on 2018 data from Liberty Mutual, BLS and the National Academy of Social Insurance, estimated direct costs to employers (medical and lost- wage payments) of injuries resulting in cases involving five or more days of lost time. If indirect costs also are considered, the overall costs are much higher. Based on calculations used in the previous Liberty Mutual Safety Index, the data indicate that businesses pay between $176 billion and $352 billion annually in direct and indirect (overtime, training and lost productivity) costs on workers’ compensation losses for the most disabling injuries (indirect costs are estimated to be two to five times direct costs).²⁰ It is important to note that the safety index excludes a large number of injury cases (those resulting in less than five days of lost time). In addition, Liberty Mutual bases its cost estimates on BLS injury data. Thus, all the problems of underreporting in the BLS system apply to the Liberty Mutual cost estimates as well.
A 2011 comprehensive study examined a broad range of data sources, including data from the BLS, the Centers for Disease Control and Prevention (CDC), the National Council on Compensation Insurance and the Healthcare Cost and Utilization Project, to determine the cost of fatal and nonfatal occupational injuries and illnesses for 2007. This study estimated the medical and indirect (productivity) costs of workplace injuries and illnesses at $250 billion annually, more than the cost of cancer.²¹ A follow-up analysis found that workers’ compensation covered only 21% of these costs, with 13% borne by private health insurance, 11% by the federal government and 5% by state and local governments. Fifty percent of the costs were borne by workers and their family members.²²
A 2015 report by OSHA—“Adding Inequality to Injury: The Costs of Failing to Protect Workers on the Job”—outlined how work-related injuries have devastating impacts on workers and their families. According to the report, workers who are injured on the job suffer great economic loss. Even after receiving workers’ compensation benefits, injured workers’ incomes are, on average, nearly $31,000 lower over 10 years than if they had not suffered an injury.²³
One of the major contributors to the severe loss of income is the gross deficiencies and inequities in the workers’ compensation system, which continues to be governed by 50 different state laws.
A 2015 multipart series by Pro Publica and National Public Radio exposed the failure of the workers’ compensation system to provide fair and timely compensation for workers hurt on the job.²⁴ The series—“Insult to Injury: America’s Vanishing Worker Protections”—was based on a yearlong investigation, which found that over the previous decade there had been a systematic effort by insurers and employers to weaken workers’ compensation benefits for injured workers. Since 2003, legislators in 33 states have passed legislation reducing benefits or limiting eligibility. The benefits provided to workers vary widely. For example, at the time of the investigation, the maximum compensation for loss of an eye was $261,525 in Pennsylvania, but only $27,280 in Alabama. In many states, employers have great control over medical decisions. Workers are not allowed to pick their own doctors, and employers can demand review by “independent medical examiners” picked by employers who can challenge medical determinations regarding the work-relatedness of the condition, the degree of disability and prescribed treatment. According to Pro Publica, all of these factors have contributed to the demolition of the workers’ compensation system and left injured workers and their families, and society at large, bearing the costs of their injuries.
19 2021 Liberty Mutual Workplace Safety Index. Available at Business.LibertyMutual.com/wp- content/uploads/2021/06/2021_WSI_1000_R2.pdf.
20 Liberty Mutual Research Institute for Safety, news release, April 16, 2002.
21 Leigh, J.P. “Economic Burden of Occupational Injury and Illness in the United States.” The Milbank Quarterly
89, No. 4. December 2011. Available at doi.org/10.1111/j.1468-0009.2011.00648.x.
22 Leigh, J.P., and J. Marcin. “Workers’ Compensation Benefits and Shifting Costs for Occupational Injuries and Illnesses.” Journal of Occupational and Environmental Medicine 54, No. 4. April 2012. Available at 10.1097/JOM.0b013e3182451e54.
23 U.S. Department of Labor, Occupational Safety and Health Administration. “Adding Inequality to Injury: The Costs of Failing to Protect Workers on the Job.” 2015. Available at OSHA.gov/sites/default/files/inequality_michaels_june2015.pdf.
24 Pro Publica and National Public Radio. “Insult to Injury: America’s Vanishing Worker Protections.” March 2015. Available at ProPublica.org/series/workers-compensation.
Demographics
Women Workers
In 2020, 387 women died on the job, compared with 4,377 men, who often work in more dangerous industries. However, in 2020, a larger percentage of women died in the workplace due to exposure to harmful substances or environments than men (15% of all workplace fatalities for women compared with 14% for men) and homicide (17% compared with 7%). Workplace homicides were the second-leading cause of workplace job death for women workers. Domestic violence in the workplace has become a worsening problem; women were more than 50% more likely to be killed by a relative or domestic partner at work than men.
In 2020, women suffered 585,540 serious lost-time injuries and illnesses, 1.3% higher than men. These numbers included COVID-19 illnesses that have been reported. Women nursing assistants, orderlies and psychiatric aides; registered nurses; laborers and material movers; and building cleaning workers had the highest numbers of serious injuries in 2020. Women were at much greater risk of injuries from workplace violence, experiencing seven of every 10 serious injuries.
Aging Workers
Workers 65 and older have 2.5 times the risk of dying on the job than all workers, with a fatality rate of 8.6 per 100,000 workers in 2020. Workers ages 55–64 also are at increased risk, with a fatality rate of 4.4 per 100,000 workers. In 2020, 38% of all fatalities (1,727 deaths) occurred in workers ages 55 years and older, with 676 of these deaths occurring in workers ages 65 years and older. People are working longer, and by 2030, all baby boomers will be 66 years and older, and one in four workers will be 65 years and older.²⁵
²⁵ Bureau of Labor Statistics. “Employment Projections Overview and Highlights—2020–30” (press release). Sept. 8, 2021. Available at BLS.gov/news.release/pdf/ecopro.pdf.
Racial Disparities
The fatality rate among Latino workers (4.5 per 100,000) increased for the second year in a row and has increased 15% over the past decade. The Latino fatality rate is 32% higher than the overall job fatality rate of 3.4 per 100,000 workers. The job fatality rate for Latino workers peaked in 2001 at 6.0 per 100,000 workers.
Latino worker deaths slightly decreased in 2020 to 1,072 deaths. This is following a drastic increase in Latino worker deaths immediately leading up to the pandemic: 1,088 Latino workers died on the job in 2019, an increase from 961 in 2018 and 903 deaths in 2017. In 2020, 269 Latino workers died from falls, slips or trips, compared with 267 in 2019 and 190 in 2018. In 2020, 170 Latino workers died from exposure to harmful substances or environments, a 14% increase from 2019 (149). Of the 1,072 Latino workers killed on the job in 2020, 65% were born outside of the United States.
Black workers face an increased risk of work-related deaths, with a job fatality rate of 3.5 per 100,000 workers, a decrease from 3.6 in 2019 but the second year in a row the fatality rate for Black workers is greater than the overall job fatality rate of 3.4. In 2020, 541 Black workers died—down from 634 in 2019, the highest number seen in more than two decades.. In 2018, 615 Black workers died on the job and 530 Black workers died on the job in 2017. The number of Black deaths due to violence on the job (125) decreased from 162 in 2019.²⁶
The number of serious work injuries and illnesses increased for all races in 2020 and included illnesses from COVID-19. The number of serious work injuries and illnesses in all industries among Asian workers increased 70% in 2020 (from 13,730 to 23,420). Serious work injuries and illnesses increased 40% among Black workers (from 89,360 to 125,350), 27% among Hispanic or Latino workers (from 139,790 to 177,290) and 22% among White workers (from 369,660 to 450, 820).
In 2020, the Bureau of Labor Statistics updated its disclosure methodology resulting in significantly fewer publishable data for immigrants—leading to less transparency about a significant number of workplace deaths in the United States. This has resulted in previously published data by state, country and gender no longer being available for Latino workers, as well as occupation, industry and other information no longer being available for many other immigrant workers.²⁷ Fatalities among all foreign-born workers continue to be a serious problem. Targeted OSHA enforcement and training programs in workplaces and industries with greater density of Latino and immigrant workers have been effective at reducing job fatalities and improved working conditions. The Obama administration instituted these programs, yet they have not been carried forward through other administrations.
²⁶ Excludes animal-related violence incidents.
Regulatory Action and Reform
Twice a year, the president publishes a regulatory agenda for each agency to set its regulatory priorities for the next six months. The most recent agenda was published by the Biden administration in Fall 2021. Pre-rulemaking priorities include workplace violence in health care and social assistance, heat illness prevention in indoor and outdoor work settings, and emergency response. Rulemaking priorities include powered industrial trucks, hazard communication updates, welding in construction confined spaces, infectious disease, tree care, updates to the lock-out tag-out standard, and communications towers.
The agency’s long-term agenda includes the restoration of the column for employer recording of musculoskeletal disorders (MSDs) onto the OSHA injury and illness log, receiving little attention by the agency despite accounting for the largest (21%) of all serious nonfatal workplace injuries. The agency issued a proposed rule on this in 2010, but withdrew it in 2011. Initially, the 2001 final recordkeeping rule had included an MSD column, but OSHA later deleted that column before the provision became effective.
Thus far, this administration has completed a small business review for emergency response and issued proposed rules on powered industrial trucks and electronic injury reporting.
The issuance of a proposed rule on electronic injury reporting would restore requirements for large employers to submit detailed injury information to OSHA, which was revoked by the Trump administration in 2019. On March 30, 2022, the Biden administration proposed to reinstate these requirements.²⁸
OSHA issued an electronic injury reporting rule in May 2016 that included provisions prohibiting retaliation against workers for reporting injuries, and making such actions a regulatory violation subject to citation and penalties (29 CFR 1904.35). The anti-retaliation provisions became effective in December 2016 and remain in effect. In January 2019, the Trump administration revoked the requirement for large employers to submit detailed injury information.
There are still many priorities on the regulatory agenda that have not yet seen progress publicly. One includes a proposed rule to protect communications tower workers. Communications tower climbers install, maintain and repair equipment at significant heights, in rural and urban areas, and in all weather conditions. The majority of these workers are contract workers employed in small contracting firms scattered throughout the nation. They face such hazards as falls, extreme weather, animal attacks, Lyme disease, mosquito-borne illnesses, radiofrequency radiation. Over the past five years, there have been at least 33 reported deaths at wireless tower sites. Of the fatalities investigated by OSHA over the most recent five years, the agency issued 44 violations for a total penalty of $367,500 against tower contractors.²⁹ As noted in the overview of fatalities, there is less transparency of contract worker deaths than there has been over the past decade due to a recent BLS disclosure policy.
Regulatory “reform” bills have been a problem over the years, introduced by conservatives. Despite the name, these bills would make it more difficult or impossible for agencies to issue needed safeguards in a timely manner. The most recent of these bills is the Setting Manageable Analysis Requirements in Text Act (S. 2801), creating unnecessary, redundant requirements that would shift resources away from the development and issuance of public protections, including important job safety and health standards. Similar bills over the years have had different titles but add new requirements for OSHA and other agencies to get protections out the door. Over the years, OSHA’s standard-setting process has become unduly burdensome and lengthy. According to a congressional report, it takes OSHA between 4.3 and 11.5 years to issue a new standard―an average of eight years.³⁰ The most time OSHA has taken to complete the rulemaking process was 19 years each for the two most recent chemical standards—silica and beryllium.
28 See FederalRegister.gov/documents/2022/03/30/2022-06546/improve-tracking-of-workplace-injuries-and- illnesses.
29 See WirelessEstimator.com/content/fatalities.
30 Congressional Research Service. “Occupational Safety and Health Administration (OSHA): COVID-19 Emergency Temporary Standards (ETS) on Health Care Employment and Vaccinations and Testing for Large Employers.” Updated March 24, 2022. Available at CRSReports.congress.gov/product/pdf/R/R46288.
OSHA Enforcement and Oversight
Enforcement is a cornerstone of the Occupational Safety and Health Act and always has been a major part of the OSHA program. However, different administrations have placed different levels of emphasis on enforcement. In general, Democratic administrations have favored strong enforcement, supplemented by compliance assistance and voluntary programs, while Republican administrations have placed a greater emphasis on compliance assistance and lesser on enforcement. But all administrations face deficiencies and weaknesses in OSHA’s statutory enforcement authority, and significant resource constraints that have greatly limited the agency’s ability to meet its responsibilities.
For the entire four-year term of the Trump administration, OSHA did not have a confirmed head of the agency. Enforcement did not change significantly for the first two years; however, enforcement policy changes in 2019 shifted the focus of OSHA inspections to emphasize quantity rather than significant inspections. The number of onboard OSHA inspectors declined significantly due to President Trump’s federal hiring freeze and the failure to fill vacant positions. As a result, the overall level of enforcement activity, particularly involving more complicated and time-intensive cases, declined.
Since taking office, the Biden administration’s OSHA has responded to several major workplace safety incidents. In late January, a liquid nitrogen leak at a Georgia poultry plant killed at least six people, sent a dozen to the hospital and forced the plant to evacuate; many of these workers were Latino and immigrants.31 In Florida, an investigation into a lead smelter is expected to be significant as the employer is allowing toxic occupational lead exposures; many of these workers are Black or immigrants.32
The OSH Act excluded many workers from coverage, including workers covered by other safety and health laws, and state and local public employees in states without a state OSHA plan. Over the years, there have been efforts to expand coverage. But today millions of workers—many state and local public employees—still lack OSHA coverage and are at much greater risk of being injured on the job.
OSHA Inspections
Federal OSHA’s ability to provide protection to workers has greatly diminished over the years. When the AFL-CIO issued its first “Death on the Job: The Toll of Neglect” report in 1992, federal OSHA could inspect workplaces under its jurisdiction once every 84 years, compared with once every 236 years under current staffing and inspection levels; however, OSHA did not conduct as many inspections across the board in 2021 and 2020, during the COVID-19 pandemic. In 2019, pre-pandemic, this figure was 162 years.
In FY 2021, federal OSHA conducted 24,355 inspections, and the state OSHA agencies combined conducted 31,063 inspections. This was a significant decrease from past years due to reduced enforcement activity during the COVID-19 pandemic; a 27% reduction for federal OSHA and a 26% reduction for state OSHA agencies compared with FY 2019.
For the first time, inspection data in federal agencies was requested and provided by federal OSHA. In FY 2021, federal OSHA conducted 604 inspections in federal agencies, including 160 inspections at the Department of Defense, 68 at the Department of Interior, 115 at the Veterans Administration and 60 at the Department of Agriculture.
There has been a decline in enforcement activity involving significant and complicated cases that began during the Trump administration and can be seen in the data from OSHA’s Enforcement Weighting System (EWS)—a protocol implemented under the Obama administration that gives greater weight to more time-intensive inspections than to shorter duration routine inspections, and under the OSHA Weighting System (OWS)—a protocol initiated under the Trump administration that downgrades complex health inspections with significant importance and impact, and increases the weight of quick inspections related to four fatal safety hazards (falls, caught in, struck by and electrical hazards).33
Both systems assign different weights to different types of inspections performed by OSHA compliance safety and health officers. The change to the newer OWS system during the Trump administration masked the significant decrease in these inspections.
Under the EWS, in FY 2019, OSHA reported 42,825 enforcement units (EUs) for inspections and investigations, compared with 42,900 EUs in FY 2016, despite more inspections being conducted in FY 2019 (33,401 from 31,948). From FY 2016 to FY 2019, the number of inspections for significant cases declined from 131 to 100 (a 24% decline); the number of inspections for ergonomic hazards declined 55%, from 69 to 31; the number of inspections for workplace violence declined 29%, from 49 to 35; the number of inspections for process safety management declined 26%, from 234 to 172; and the number of inspections for combustible dust declined 24%, from 491 to 372.
In FY 2021, OSHA reported 48,271 EUs for inspections and investigations, compared with 43,217 EUs for inspections and investigations in FY 2020. These cannot be compared with the EWS EUs; however, a critical examination of the OWS EUs shows the difference is striking. Under the OWS, the majority of EUs result from inspections related to the fatal four safety hazards, 24,246 of 48,271 EUs in FY 2021. However, EUs resulting from inspections from ergonomics, heat, non-PEL overexposures and workplace violence combined only accounted for 82 of 48,271 EUs in FY 2021. This new system masks the number of health inspections completed and disincentivizes inspectors from completing time intensive and complex, yet significant, health inspections—the opposite intended effect of the original weighting system.
The system has not changed under the Biden administration.
Unprogrammed Enforcement Activity
OSHA refers to enforcement activity that isn’t due to an enforcement directive, nonprogrammed activity. This includes enforcement activity due to complaints, referrals, employer-required severe injury reports, and fatality and catastrophe investigations. This is the first year the AFL- CIO has requested this data.
Individuals can file a complaint with OSHA that an employer is not providing a safe workplace. The agency considers a complaint as “formal” if it is made by a current employee or representative that asserts imminent danger or a violation of the OSH Act or a standard. Formal complaints must be written or use OSHA’s complaint form, and must be signed. Other complaints that do not meet that criteria are considered “informal.” In FY 2021, federal OSHA received 4,549 formal complaints and 21,197 informal complaints. Federal OSHA inspected the workplace in 44% of formal complaints and 16% of informal complaints. State plan OSHAs received 9,723 formal complaints, inspecting 50%, and 37,333 informal complaints, inspecting 10%. Complaints that did not receive an inspection results in the agency doing a “phone/fax investigation.” When conducting a phone/fax investigation, the agency telephones the employer, describes the alleged hazards in the complaint and then follows up with a letter. The employer must respond within five days, identifying in writing any problems found and noting corrective actions taken or planned. If OSHA determines the response adequate, an on-site inspection is not conducted. Phone/fax investigations were formerly only conducted in response to an informal complaint, but this practice changed during the COVID-19 pandemic to allow inspectors to conduct phone/fax investigations for all types of unprogrammed activity.
In FY 2021, federal OSHA received 3,696 referrals and responded with an inspection for 64% after referral. State OSHA plans received 12,285 referrals and followed up by inspecting 47%. OSHA inspectors, other federal, state or local government agencies, discrimination or whistleblower complaints or the media can refer a case to OSHA.
In 2015, OSHA began requiring employers to report all severe work-related injuries, defined as an amputation, in-patient hospitalization or loss of an eye, to the agency. In response to these reports, the agency conducts either an inspection or rapid response investigation (RRI). An RRI does not involve an on-site inspection, and requires the employer to conduct its own investigation into the incident and share their findings with OSHA. In FY 2021, federal OSHA received 10,422 severe injury reports (SIRs) and conducted an inspection in 30% of cases, and state plan OSHAs received 3,365 SIRs and conducted an inspection in 47% of cases.
Federal OSHA received reports of 2,831 fatalities and catastrophes on the job in FY 2021 and investigated 55% of the cases. State OSHA received reports of 12,079 fatalities and catastrophes and investigated 37%.
OSHA Violations and Penalties
Penalties for OSHA violations have always been relatively low, due to statutory limitations and enforcement policies that prioritize the settlement of cases in order to achieve quicker abatement of hazards, rather than imposing the maximum fines.
In recent years, administrative and statutory changes have resulted in an increase in OSHA penalties. A revised penalty policy implemented during the Obama administration in 2010 resulted in a doubling of fines for serious violations. Passage of the Federal Civil Penalties Inflation Adjustment Act Improvements Act of 2015, which extended the coverage of the Inflation Adjustment Act to OSHA, further increased penalties for OSHA violations. Under the 2015 law, OSHA was authorized to raise maximum penalties by approximately 80%, the amount of inflation since the last time OSHA penalties were raised in 1990, and to regularly update penalties to account for future inflation.
This statutory increase in federal OSHA penalties took effect Aug. 1, 2016. The latest adjustment, effective Jan. 14, 2022, increased the maximum penalty for serious violations to $14,502, and for willful and repeat violations to $145,027.34,35,36 State OSHA plans also are required to raise their statutory maximum penalties in order to be as effective as the federal OSHA program, but many states that cover private sector workers have not yet complied. As of April 15, 2022, only 12 of 24 states have adopted increased penalties: Alaska, California, Hawaii, Iowa, Nevada, New Mexico, Oregon, Utah, Virginia, Vermont, Washington and Wyoming. (Connecticut, Illinois, Maine, New Jersey and New York, which only cover public sector workers, are not required to.)37
In FY 2021, the average penalty for a serious violation under federal OSHA was $4,460, compared with an average penalty of $3,923 for serious violations in FY 2020. In FY 2021, the average penalty for a serious violation for state OSHA plans combined remained lower, at $2,421; in FY 2020, it was $2,137.
The number of willful violations cited by federal OSHA in FY 2021 was 360, a decrease from FY 2020. The average penalty per willful violation was $61,750 in FY 2021, compared with $70,797 in FY 2020 and $59,373 in FY 2019. The average penalty per repeat violation was $13,277 in FY 2021, compared with $15,340 in FY 2020. In states with state-run OSHA plans, in FY 2021, there were 518 willful violations issued, with an average penalty of $27,312 per violation, and 2,139 repeat violations issued, with an average penalty of $5,203 per violation.
In FY 2021, federal OSHA issued 636 violations to federal agencies, including one willful violation and 68 repeat violations. Federal OSHA does not issue monetary penalties as a result of violations to federal agencies.
For FY 2020, federal OSHA reported that the agency brought 65 “significant” enforcement cases.38 This is fewer than FY 2020 (89) and more than the first year of the Trump administration, FY 2017 (53).39 It is unclear how significant enforcement cases may have been impacted by the COVID-19 pandemic and reduction in enforcement activity.
The median current penalty issued per fatality investigation conducted in FY 2021 was $9,753 for federal OSHA and the median current penalty was $5,825 for the state OSHA plans combined, according to enforcement data provided by OSHA in March 2022. This compares with the respective penalties in FY 2020: $12,144 for federal OSHA and $6,899 for the state OSHA plans combined. These data include enforcement cases that still are under contest, and some cases that still are open. Increased penalties in FY 2021 and FY 2020 may be attributed to a combination of Congress tying maximum penalties to inflation annually and the COVID-19 pandemic: in the COVID-19 pandemic, OSHA has continued to conduct fewer total inspections and issue fewer citations than OSHA typically issues in a fiscal year. The pandemic created a smaller pool of data in total and inspections were focused on COVID-19, rather than the many safety and other hazards OSHA typically cites throughout the year.
Averages can distort the real picture of fatality penalties in situations in which large cases with very high penalties raise the averages substantially. Using median penalties that capture the point where half of the penalties are below and half the penalties are above the median provides a more accurate picture of the typical penalties in cases involving worker deaths. According to OSHA inspection data, the average total penalty in a fatality case in FY 2021 was just $11,626 for federal and state OSHA plans combined.
OSHA Enforcement Initiatives and Policies
Throughout the Trump administration, and in the four-year absence of a confirmed assistant secretary, there was only one major overhaul or reorientation of OSHA’s enforcement program. A number of enforcement programs and initiatives implemented by the Obama administration continued. However, key policies and practices implemented by the Obama administration to enhance worker rights and improve transparency and disclosure were rolled back.
In response to calls from the business community, the Trump administration in April 2017 withdrew the Obama administration’s policy that provided for nonunion workers to designate a walkaround representative to participate on their behalf in OSHA worksite inspections. The policy, set forth in a 2013 letter of interpretation, clarified that under OSHA regulations, a collective bargaining representative or another individual designated by the employees, if the inspector determined the individual would aid the inspection, could serve as the walkaround representative.40 This provided for nonunion workers to designate a union or worker center as their representative for the purpose of participating in the OSHA inspection. Business groups strongly objected to and challenged this policy. In response, the Trump administration withdrew this letter of interpretation, stating it no longer represented OSHA policy.
The Trump administration also backtracked on Obama administration initiatives to use public disclosure of information to highlight serious safety and health problems. In 2010, OSHA started posting information on every fatality report it received on the home page of its website, to educate and inform the public about the high toll of work-related deaths and the need to prevent them. The information included the name of the worker, the circumstances surrounding the death and the employer. In August 2017, the Trump administration stopped posting these reports.
OSHA reported only fatalities it investigated and, citing privacy concerns, would not release the name of the deceased worker. Worker fatality information no longer was posted on the home page of OSHA’s website, which instead displayed initiatives OSHA was taking to cooperate with employers. Families of workers killed on the job protested this change in policy, which diminished attention to these workplace deaths.
The Obama administration also expanded the use of press releases on significant enforcement cases to focus public attention on employers with serious, willful or repeated violations of the law. OSHA had always issued press releases on important enforcement cases, but under the Obama administration, it was OSHA policy to issue a press release on all enforcement cases with total proposed penalties of greater than $40,000, and for local OSHA officials to engage in active outreach to the press. A recent study found that one OSHA press release was the equivalent of 210 inspections, an essential compliance assistance tool given limited agency resources.41 The business community strenuously objected to the issuance of these press releases, and when the Trump administration took office, the issuance of OSHA press releases on enforcement cases was suspended. Several months later, from public pressure, the agency again issued some press releases for some major enforcement cases, but there no longer was a policy or practice to issue press releases on all significant enforcement cases. Press releases have resumed under the Biden administration.
Other Obama administration programs and policies to address high-hazard employers and industries and to respond to changes in the workforce and employment relationships have continued. These include the Severe Violator Enforcement Program, launched in 2010, to focus on and provide enhanced oversight of the most persistent and egregious violators; the Temporary Worker Initiative (TWI) to help prevent injuries and illnesses among temporary workers by holding both staffing agencies and host employers jointly responsible; and the Severe Injury Reporting and Investigation Program.
According to OSHA, 68 new cases were added to the log of the Severe Violator Enforcement Program in FY 2020. As of the end of FY 2020, 702 employers remained in the severe violator program subject to OSHA enforcement.42
OSHA has continued to conduct the Temporary Worker Initiative to help prevent injuries and illnesses among temporary workers who are employed by staffing agencies but who work for different host employers. However, the number of inspections conducted under the TWI have declined significantly. Under OSHA’s temporary worker policy, both host employers and staffing agencies may be held jointly responsible for complying with safety and health rules.
The Biden administration issued several new enforcement directives and national emphasis programs to address the urgent issues of COVID-19 and heat to help protect workers from these hazards while the administration moves through the rulemaking process.43,44,45,46
State Plan Oversight
The OSH Act permits federal OSHA to grant approval to states that want to manage their own workplace safety and health program and cover public sector workers in their states. One stipulation for approval, however, is that the states’ safety standards are “at least as effective” as federal standards. State standards can be stricter than federal OSHA’s standards but not weaker. When states are clearly not fulfilling their duty to be at least as effective as federal OSHA, there are limited options for federal OSHA to step in.
Federal OSHA’s main tool is to remove the state’s OSHA state plan approval. The process to approve or revoke a state plan requires a lengthy rulemaking process, including public comment. This also has two significant side effects. If federal OSHA went through with revoking a state plan, federal OSHA would be in charge of all enforcement in the state, adding to its responsibilities while not gaining resources, and public employees would lose OSHA coverage provided to them through their state plan.
Two recent examples discussed elsewhere in this report of this malfeasance are not adopting updated penalty maximums and being slow or, in the case of Arizona, never adopting the COVID-19 ETS for health care, leaving many workers unprotected. In the latter case, federal OSHA sent “courtesy letters” to the state plans that were slow to adopt and placed a proposed rule to revoke approval of Arizona’s state plan on its regulatory agenda. To date, no proposed rule has been issued.
Previously, OSHA has had some success in ensuring state plans adopt rules or run programs at least as effective as federal OSHA. During the Obama administration, federal OSHA threatened to withdraw South Carolina’s state plan when the state announced it was going to eliminate its OSHA whistleblower program. The state finally relented, largely at the urging of South Carolina’s business community.
OSHA Criminal Enforcement
Throughout OSHA’s history, criminal enforcement under the Occupational Safety and Health Act has been rare and dependent on political will. According to information provided by the Department of Labor, since the passage of the act in 1970, only 115 cases have been referred for prosecution under the act. During this time, there were approximately 425,000 workplace fatalities. In FY 2021, DOL referred nine cases for criminal prosecution, compared with seven cases in FY 2020, four cases in FY 2019, 11 cases in FY 2018 and 19 cases in FY 2017. 47, 48,49
By comparison, the Environmental Protection Agency reported in FY 2021 that there were 123 criminal enforcement cases initiated under federal environmental laws—and in 88% of the criminal cases charged, an individual defendant was prosecuted, and those prosecutions generated a total 96% conviction rate.50 The aggressive use of criminal penalties for enforcement of environmental laws, and the real potential for jail time for corporate officials, serve as a powerful deterrent.
The criminal penalty provisions of the OSH Act are woefully inadequate. Criminal enforcement is limited to those cases in which a willful violation results in a worker’s death, or where false statements in required reporting are made. The maximum penalty is six months in jail, making these cases misdemeanors. Criminal penalties are not available in cases where workers are endangered or seriously injured, but no death occurs. This is in contrast to federal environmental laws, where criminal penalties apply in cases where there is “knowing endangerment,” and the law makes such violations felonies. Due to the weak criminal penalties under the OSH Act, the Department of Justice (DOJ) prosecutes few cases under the statute. Instead, in some instances, DOJ will prosecute OSHA cases under other federal statutes with stronger criminal provisions if those laws also have been violated.
In response to the OSH Act’s severe limitations, over the years there have been a number of initiatives to expand criminal enforcement for safety and health hazards by utilizing other statutes for prosecution. These include the DOJ Worker Endangerment Initiative, launched in 2005 and expanded in 2016, that focuses on companies that put workers in danger while violating environmental laws, and prosecutes such employers using the much tougher criminal provisions of environmental statutes.51, 52, 53 Under this initiative, DOJ has significantly enhanced its criminal prosecutions for worker safety and health, successfully bringing cases that have resulted in convictions and significant jail time for defendants.54 During the Obama administration, the Department of Labor (DOL) stepped up criminal enforcement efforts, referring more cases for criminal prosecution to the DOJ and U.S. attorneys. In addition, DOL expanded assistance to local prosecutors in the investigation and prosecution of cases involving worker deaths and injuries.
While criminal enforcement of job safety violations at the federal level remains quite limited, in a number of states and localities, prosecutors are pursuing criminal charges against employers and individuals in cases involving job deaths and injuries. In Philadelphia, the district attorney successfully prosecuted the general contractor and crane operator for deaths of six individuals in the 2013 Salvation Army building collapse, winning convictions for involuntary manslaughter and jail time. In New York City, the Manhattan district attorney won a manslaughter conviction against the general contractor, Harco Construction, for the 2015 trenching death of a young undocumented immigrant construction worker. The foreman for the excavation company, Sky Materials, was convicted of criminally negligent homicide and reckless endangerment, and sentenced to one to three years in jail. In both cases, unions and local safety and health activists worked with prosecutors to provide assistance and to educate the community about the job safety crimes.
OSHA Coverage
OSHA law still does not cover 7.9 million state and local government employees in 24 states and the District of Columbia, although these workers encounter the same hazards as private sector workers, and in many states, have a higher rate of injury than private sector counterparts.55,56 Similarly, millions who work in the transportation and agriculture industries and at Department of Energy contract facilities lack full protection under the OSH Act. These workers theoretically are covered by other laws, which in practice have failed to provide equivalent protection. The Mine Safety and Health Administration (MSHA) covers many underground and surface mine workers under its own law, which is stronger than the OSH Act.
In 2013, OSHA coverage was extended to flight attendants when the Federal Aviation Administration rescinded a longstanding policy and ceded jurisdiction to OSHA on some key safety and health issues, in response to the FAA Modernization and Reform Act of 2012 (PL 112-95). This policy action was the culmination of decades of effort by the flight attendant unions to secure OSHA protections. Specifically, the FAA issued a policy that extended OSHA regulations and jurisdiction on hazard communication, bloodborne pathogens, hearing conservation, recordkeeping, and access to employee exposure and medical records for cabin crews.57
The COVID-19 pandemic continues to highlight the consequences of inadequate OSHA coverage in workplaces across the country. OSHA has not reached many workplaces to ensure workers are protected.
Years Needed for OSHA to Inspect All Job Sites (PDF)
Years for Federal OSHA to Inspect Each Workplace Once (PDF)
Federal OSHA and State Plan OSHA Inspection/Enforcement Activity, FY 2021 (PDF)
Number of Federal OSHA Inspections by Industry (PDF)
Federal OSHA Enforcement Activity Addressing Significant Hazards, FY 2021 (PDF)
Federal OSHA Inspection/Enforcement Activity in Federal Agencies, FY 2020–2021 (PDF)
Average Total Penalty Per OSHA Fatality Inspection, FY 2014–2021 (PDF)
State-by-State OSHA Fatality Investigations, FY 2021 (PDF)
Significant OSHA Enforcement Cases Based on Total Penalty Issued, FY 2021 (PDF)
7.9 Million State and Local Employees Lacked OSHA Coverage in 2020 (PDF)
32 See Projects.TampaBay.com/projects/2021/investigations/lead-factory/gopher-workers/.
33 See OSHA.gov/sites/default/files/CTS_7132_Whitepaper_FINAL_v2019_9_30.pdf. Effective Sept. 30, 2019.
34 Prior to the passage of the Federal Civil Penalties Inflation Adjustment Act Improvements Act of 2015, the maximum penalty for a serious violation was $7,000 and the maximum penalty for a willful or repeat violation was $70,000 per violation.
35 See FederalRegister.gov/documents/2022/01/14/2022-00144/department-of-labor-federal-civil-penalties-inflation-adjustment-act-annual-adjustments-for-2022. Jan. 14, 2022.
36 See OSHA.gov/memos/2022-01-13/2022-annual-adjustments-osha-civil-penalties. Jan. 13, 2022.
37 Information compiled by the OSHA Directorate of Cooperative and State Programs, updated April 15, 2022. Utah adoption will be in effect May 4, 2022.
38 OSHA defines a significant enforcement case as one where the investigation results in a total proposed penalty of greater than or equal to $180,000, or one that involves novel enforcement issues.
39 For the first 10 months of FY 2016, the threshold for a significant case was $100,000; it increased to $180,000 on Aug. 1, 2016, when the increase in maximum penalties took effect.
40 Fairfax, Richard E., Deputy Assistant Secretary, Occupational Safety and Health Administration, Letter to Steve Sallman, Health and Safety Specialist, United Steel, Paper and Forestry, Rubber, Manufacturing, Energy, Allied Industrial and Service Workers International Union (USW). Feb. 21, 2013. Available at OSHA.gov/laws- regs/standardinterpretations/2013-02-21.
41 Johnson, M.S. “Regulation by Shaming: Deterrence Effects of Publicizing Violations of Workplace Safety and Health Laws.” American Economic Review 110 (6):1866–1904. June 2020. Available at 10.1257/aer.20180501. 42 OSHA Inspection Data in Response to AFL-CIO Data Request, FY 2021.
43 OSHA. Updated Interim Enforcement Response Plan for Coronavirus Disease 2019 (COVID-19). July, 7, 2021. Accessed at OSHA.gov/laws-regs/standardinterpretations/2021-07-07.
44 OSHA Directive: DIR 2021–03 (CPL 03). Revised National Emphasis Program – Coronavirus Disease 2019 (COVID-19). July 7, 2021. Accessed at OSHA.gov/sites/default/files/enforcement/directives/DIR_2021- 03_CPL_03.pdf.
45 COVID-19 Focused Inspection Initiative in Healthcare. March 2, 2022. Accessed at OSHA.gov/laws- regs/standardinterpretations/2022-03-02.
46OSHA Directive: CPL 03-00-024. National Emphasis Program – Outdoor and Indoor Heat-Related Hazards. April 8, 2022. Accessed at OSHA.gov/sites/default/files/enforcement/directives/CPL_03-00-024.pdf.
47 “Criminal Referrals by OSHA to DOJ or US Attorneys or Significant Aid to Local Prosecutors (Updated April 8, 2016)” and other information compiled and provided by the Office of the Solicitor of Labor, updated April 11, 2022. The information for the early years of the statute is incomplete and may not include all cases prosecuted.
48 In addition to cases prosecuted under the Occupational Safety and Health Act and the U.S. federal criminal code (18 U.S.C. 1001), state and local prosecutors have prosecuted employers for deaths and injuries to workers under their state and local laws. There is no complete accounting of these cases.
49 Information on criminal referrals provided by the U.S. Department of Labor, Office of the Solicitor of Labor. 50 U.S. Environmental Protection Agency. Enforcement Annual Results for Fiscal Year 2021. Available at EPA.gov/enforcement/enforcement-annual-results-fiscal-year-
2021#:~:text=In%20FY%202021%2C%20EPA's%20enforcement,communities%20with%20environmental%20justi ce%20concerns.
51 Goldsmith, A.D. “Worker Endangerment Initiative.” PowerPoint presentation, American Bar Association, Occupational Safety and Health Committee, Miami Beach, Florida. February 2009.
52 Department of Justice, Office of Public Affairs. “The Departments of Justice and Labor Announce Expansion of Worker Endangerment Initiative to Address Environmental and Worker Safety Violations” (press release). Dec. 17, 2015. Available at Justice.gov/opa/pr/departments-justice-and-labor-announce-expansion-worker-endangerment- initiative-address.
53 Memorandum of Understanding between the U.S. Departments of Labor and Justice on Criminal Prosecutions of Worker Safety Laws. Dec. 17, 2015. Available at Justice.gov/enrd/file/800526/download.
54 PBS. “Frontline: A Dangerous Business Revisited.” March 2008. Available at PBS.org/wgbh/pages/frontline/mcwane/penalty/initiative.html.
55 Under the OSH Act, states may operate their own OSHA programs. Twenty-one states and one territory have state OSHA programs covering both public and private sector workers. Connecticut, Illinois, Maine, New Jersey and New York have state programs covering state and local employees only.
56 Some states provide safety and health protection to public employees under state laws that are not OSHA- approved plans. In 2014, Massachusetts enacted legislation establishing legally binding safety and health protections for public employees, but this law has not been submitted for federal OSHA approval.
57 Department of Transportation, Federal Aviation Administration. Occupational Safety and Health Standards for Cabin Crew Members. Aug. 27, 2013. Available at FederalRegister.gov/documents/2013/08/27/2013- 20841/occupational-safety-and-health-standards-for-aircraft-cabin-crewmembers.
Whistleblower Protection
One of OSHA’s key responsibilities is to enforce the anti-retaliation provisions under section 11(c) of the Occupational Safety and Health Act. In addition, OSHA has the responsibility to enforce the whistleblower provisions of 24 other statutes, ranging from the Federal Rail Safety Act to the Sarbanes-Oxley finance law.58 Many of these statutes deal with safety and health matters, but others do not.
The total number of cases, under all statutes, received by OSHA’s whistleblower program for FY 2021 decreased from FY 2020; the number of cases completed by the agency was similar to FY 2020. In FY 2021, OSHA received 2,556 cases and completed 3,099 cases. This compares with FY 2020, when the agency received 3,448 cases—a large increase in the first year of the
COVID-19 pandemic—and completed 3,122 cases. Cases completed include cases from other fiscal years; not all cases received are completed in the same fiscal year. In FY 2021, 74% of the cases received (1,891 out of 2,556) were 11(c) complaints under the OSH Act. Workers also filed large numbers of whistleblower cases under the Federal Rail Safety Act (168), the Surface Transportation Assistance Act (202) and the Sarbanes-Oxley Act (69).59
The backlog in whistleblower cases has grown over the years and continues to be a serious problem. Adequate funding for OSHA’s whistleblower program remains a serious concern.60 The COVID-19 pandemic placed an even greater responsibility on an already starved program, limiting the agency’s ability to respond to workers alleging retaliation for raising safety concerns on the job or for wearing their own PPE when their employer did not provide it. In February 2021, OSHA was assigned two new whistleblower statutes to enforce—the Criminal Antitrust Anti-Retaliation Act and the Anti-Money Laundering Act—but has not received increased funding to carry out this additional responsibility, or resources to rebuild the program to the levels it has needed for years.
Under the Obama administration, the Department of Labor made the protection of a “worker’s voice” a priority initiative. As part of this effort, OSHA took a number of actions to strengthen the Whistleblower Protection Program to protect workers who raise job safety issues and exercise other rights from employer retaliation. The Obama administration elevated the whistleblower program, creating a new separate Directorate of Whistleblower Protection Programs at OSHA. (Previously, the program had been part of OSHA’s enforcement directorate.) To improve the timeliness and consistency of case handling, the agency updated and revised its investigators’ manual and trained staff on policies and procedures.
The Obama administration also established a Whistleblower Protection Advisory Committee composed of representatives from labor, management and the public, charged with overseeing and providing advice and guidance to OSHA on its whistleblower protection program. The Trump administration terminated this advisory committee, eliminating oversight on this important program, and held annual, generic stakeholder listening sessions instead. The Biden administration has emphasized a prioritization of vulnerable workers, equity issues and worker empowerment. It has continued the annual public whistleblower stakeholder meeting and announced hazard-specific public whistleblower stakeholder meetings on COVID-19 and heat, but it remains to be seen whether the formal advisory committee will resume and whether there will be any structural changes to the program itself.
The Obama administration created a separate budget line item for the whistleblower program and sought increased funding and staffing for the program. In its budget requests, the Trump administration proposed to reorganize the whistleblower program, eliminating the supervisory personnel for the program in the regional offices, and centralizing management and supervision for the program at OSHA headquarters in Washington, D.C. There were serious concerns that such a centralization would make it harder for whistleblower investigators in the field, who already are stretched thin, to carry out their work.
The long amount of time to resolve cases is particularly problematic under the OSH Act and those other statutes where there is no opportunity for preliminary reinstatement for workers while the case is being resolved, nor a separate right of action for the complainant to pursue the case on his or her own. During this time, workers are in limbo, with no recourse or redress for discriminatory actions. Other whistleblower statutes provide these rights.
Even with improvements in the OSHA whistleblower program in recent years, problems and deficiencies remain. The biggest problems stem from deficiencies in the OSH Act itself. The anti-retaliation provisions of the law were adopted nearly 50 years ago, and are weak and outdated compared with more recently adopted statutes. The OSH Act provides only 30 days to file a discrimination complaint, compared with 180 days provided by a number of other laws. If a worker fails to file a complaint within this time, he or she simply is out of luck, even though retaliation is not always clear in that short of a time frame, and more time often is needed to provide evidence of retaliation.
The OSH Act also has extremely limited procedures for the enforcement of discrimination cases. If there is no agreement or settlement of the findings, the secretary of labor must bring cases in U.S. District Court. Most other statutes provide for an administrative proceeding. The formal procedures of the OSH Act mean meritorious cases may be dropped simply because the solicitor of labor does not have the resources to pursue them. Moreover, unlike other statutes, such as the Mine Safety and Health Act and the Surface Transportation Assistance Act, the OSH Act does not allow a complainant the right to pursue the case on his or her own if the secretary fails to act within a designated timeframe or declines to act at all. And the OSH Act does not provide for preliminary reinstatement, as other statutes such as the Mine Safety and Health Act do, which means that workers who are retaliated against for exercising their job safety rights have no remedy while final action on their case is pending. These deficiencies in the whistleblower program can only be remedied through legislative improvements in the OSH Act.
OSHA also has addressed the issue of injury reporting through its whistleblower program—in particular, programs and policies that retaliate against workers or discourage workers from reporting injuries. In recent years, these employer programs and policies have grown in a wide range of industries. Under OSHA regulations, reporting work-related injuries is a protected activity, and employers are prohibited from retaliating against workers who report injuries. The Federal Rail Safety Act, for which OSHA enforces the whistleblower provisions, also includes specific provisions that prohibit retaliation against workers who report injuries.
To address the problems of retaliation related to injury reporting, in March 2012 OSHA issued a policy memorandum to provide guidance to the field.61 The memo outlined the types of employer safety incentive and disincentive policies and practices that could constitute illegal retaliation under Section 11(c) and other whistleblower statutes, and the steps investigators should take in responding to complaints of employer retaliation for injury reporting. To date, the memo remains in effect.
In October 2018, OSHA issued an enforcement memo that limited the scope of anti-retaliation protections when employers report injuries, as they apply to workplace safety incentive programs and post-incident drug testing, placing the burden on workers to demonstrate actual retaliation in individual cases, rather than creating a presumption that certain types of programs were impermissible.62 This policy interpretation greatly limits the utility of the anti-retaliation provisions in prohibiting policies and practices that discourage the reporting of injuries.
Employer groups filed legal challenges to the anti-retaliation provisions of the injury reporting rule, but the litigation was held in abeyance until the Trump administration reconsidered other aspects of the injury reporting regulation. On July 20, 2020, the U.S. District Court for the District of Columbia, under a settlement agreement, ordered OSHA to release all the worksite injury and illness reports that employers submitted on Form 300A for 2016 cases by Aug. 18, 2020.
58 See Whistleblowers.gov/sites/wb/files/2021-06/Whistleblower_Statutes_Summary_Chart_FINAL_6-7-21.pdf.
59 Occupational Safety and Health Administration. Whistleblower Investigation Data, Report Period: Oct. 1, 2020, to Sept. 30, 2021.
60 Berkowitz, D., and S. Thompson. “OSHA Must Protect COVID Whistleblowers Who File Retaliation Complaints.” National Employment Law Project. Oct. 8, 2020. Available at NELP.org/publication/osha-failed- protect-whistleblowers-filed-covid-retaliation-complaints/.
61 Richard E. Fairfax, Deputy Assistant Secretary Memorandum for Regional Administrators, Whistleblower Program Managers. “Employer Safety Incentive and Disincentive Policies and Practices.” March 12, 2012. Available at OSHA.gov/laws-regs/standardinterpretations/2012-03-12-0.
62 Kim Stille, Acting Director of Enforcement, Memorandum for Regional Administrators and State Designees. “Clarification of OSHA’s Position on Workplace Safety Incentive Programs and Post-Incident Drug Testing Under 29 CFR 1904.35(b)(1)(iv).” Oct. 11, 2018. Available at OSHA.gov/laws-regs/standardinterpretations/2018-10-11.
Job Safety Budget and Resources
Appropriations
In March 2022, Congress passed omnibus legislation that appropriated OSHA a budget of $612 million for FY 2022, a 3.4% increase from the previous year, but lower than the rate of inflation. This included slight increases for all agency sections, except for the worker training grant program that has been flat-funded since FY 2020 and for executive administration that received a slight decrease in funding. In addition, through the American Relief Plan, Congress appropriated OSHA $100 million for pandemic-related worker protection activities that must be used by the end of FY 2023. Of these funds, $10 million must be used for training grants, and not less than $5 million for COVID-19 enforcement.
The Biden administration has requested a 14.6% increase in OSHA funding for FY 2023, including a 49% increase for standards development and $2 million more for the worker training grant program.
Congress appropriated $264.5 million for mine enforcement in FY 2022 and the Biden administration requested an 11% budget increase for mine enforcement in FY 2023. In FY 2020, the budget reorganized MSHA enforcement to combine the coal mine enforcement and metal and nonmetal enforcement into one program, allocating $258.9 million for total mine enforcement. MSHA had justified this reorganization in order to use resources more efficiently, and to direct more resources to metal and nonmetal mining, which is growing, while coal mine activity continues to decline. Consolidation has reduced the targeted expertise in each of the current mine safety enforcement programs, since many inspectors come from either coal or metal and nonmetal industries, specifically. In FY 2019, the agency received $254.5 million in total for mine enforcement programs.
The National Institute for Occupational Safety and Health (NIOSH), the occupational safety and health research agency created in tandem with OSHA under the OSH Act, was appropriated
$351,800 million for FY 2022, a 2% increase from the previous year. The funding bill requires NIOSH to conduct a comprehensive surveillance study examining the industries and occupations of workers who have been infected and have died from COVID-19.
OSHA Compliance Staffing
There are currently a total of 1,719 federal and state OSHA inspectors responsible for enforcing the safety and health law at more than 10.4 million workplaces, compared with 1,798 in 2020 and 1,767 in 2019.63
The number of federal OSHA compliance inspectors declined significantly during the Trump administration, and reached its lowest level since the early 1970s, when the agency opened. As of December 2021, federal OSHA had 755 inspectors (excluding supervisors), down from 774 in 2020 and a slight increase from 746 in 2019—the lowest in the history of the agency. This reduction is the result of a combination of factors, including a federal hiring freeze imposed during the first year of the Trump administration, attrition and retirements, especially during the COVID-19 pandemic, and time required to hire new experienced inspectors.
State OSHA plans have 964 inspectors, a significant decrease from the 1,024 inspectors in 2020 and 1,021 in 2019.
The current level of federal and state OSHA inspectors provides one inspector for every 81,427 workers, compared with the benchmark of one labor inspector for every 10,000 workers recommended by the International Labor Organization for industrialized countries.64 In 17 states, the ratio of inspectors to employees is greater than one per 100,000 workers, with Arizona having the highest ratio at one inspector per 201,697 workers. Under OSHA’s current budget, the agency could spend $4.37 to protect each worker.
Since the passage of the OSH Act, the number of workplaces and number of workers under OSHA’s jurisdiction has nearly doubled, but there are fewer numbers of OSHA staff and OSHA inspectors. In 1975, federal OSHA had a total of 2,435 staff (inspectors and all other OSHA staff) and 1,102 compliance staff (including supervisors) responsible for the safety and health of 67.8 million workers at more than 3.9 million establishments. In FY 2022, there are 1,853 federal OSHA staff responsible for the safety and health of 140 million workers at more than 10.4 million workplaces. The number of workers in FY 2021 was more than a 5% decline from the previous year due to the COVID-19 pandemic.
At the peak of federal OSHA staffing in 1980, there were 2,951 total staff and 1,469 federal OSHA inspectors (including supervisors). The ratio of OSHA inspectors per 1 million workers was 14.8. But now, there are only 886 federal OSHA inspectors (including supervisors), or 5.8 inspectors per 1 million workers.
OSHA Voluntary Programs
Voluntary programs have always been part of OSHA’s compliance assistance model, but the emphasis placed on voluntary initiatives has varied under different administrations. Under the Obama administration, strong enforcement was the priority, with voluntary programs supplementing enforcement efforts. The Trump administration placed a greater emphasis on voluntary programs, while maintaining OSHA’s enforcement program. It is still too early in the Biden administration to see the effects of OSHA’s voluntary programs, but the agency has consistently spent more than 10 times the amount of money on employer compliance assistance than they have on worker training.
The major voluntary programs conducted by OSHA are the Voluntary Protection Program, a program that recognizes companies with a high level of safety and health performance, and the Alliance program, under which OSHA partners with trade associations, professional groups and others to carry out safety and health initiatives targeted at particular industries or hazards.
Alliances can be made at the national, regional or state level, with more than 1,000 alliances having been created. Currently, OSHA has 239 alliances—36 national and 203 regional/area.65 In the midst of the pandemic, where meatpacking employers were not instituting key measures to keep workers safe and OSHA was not enforcing in this industry, on June 28, 2020, federal OSHA created an alliance with the North American Meat Institute, a meatpacking industry trade association.66
63 This reflects the number of federal inspectors plus the number of inspectors “on board” reflected in the FY 2022 state plan grant applications. It does not include compliance supervisors.
64 International Labor Office. Strategies and Practice for Labor Inspection, G.B. 297/ESP/3. Geneva. November 2006. The ILO benchmark for labor inspectors is one inspector per 10,000 workers in industrial market economies.
65 See OSHA.gov/alliances.
66 See OSHA.gov/alliances/nami/nami.